Assure Health
(Assure Health Corporation)
 $898,102 committed665 investors
$898,102 committed665 investorsOFFERING TYPE: Regulation CF
PRICE PER SHARE: $1.00
VALUATION: $10.687 million
MINIMUM: $500
The “Big Idea” In 60 Seconds
The “Big Idea”
In 60 Seconds

In 1980, Bill Gates shared his vision for America: “A computer on every desk, and in every home, running Microsoft software.”
Then, on May 13th, 1986 – only six years later – Microsoft went public at $21 per share, putting the total valuation around $777 million (roughly $1.8 billion adjusted for inflation)
Today, Assure Health shares their inspiring vision for America: “A doctor in every home, at no out of pocket cost.”
Thanks to their “first-to-market” solution…
Right now, 32.4 million Americans who are on Medicare – and have supplemental coverage – can get access to daily health monitoring from a team of licensed medical providers
Better yet, a team of physicians who are not under pressure to spend less time with each patient in order to increase billings…
All at zero “out-of-pocket” costs for those who qualify!
Even better? This “Virtual Care Ecosystem” could potentially provide the U.S. Government with the “silver bullet” needed to reduce healthcare costs in America by up to tens of billions of dollars each year…
Potentially save 100,000 (or more) lives each year…
And potentially offer affordable healthcare for all — or even healthcare at no out-of-pocket cost to patients!
Getting started with Assure Health is simple, easy, and fast.

Then, on May 13th, 1986 – only six years later – Microsoft went public at $21 per share, putting the total valuation around $777 million (roughly $1.8 billion adjusted for inflation)
Today, Assure Health shares their inspiring vision for America: “A doctor in every home, at no out of pocket cost.”
Thanks to their “first-to-market” solution…
Right now, 32.4 million Americans who are on Medicare – and have supplemental coverage – can get access to daily health monitoring from a team of licensed medical providers.
Better yet, a team of physicians who are not under pressure to spend less time with each patient in order to increase billings…
All at zero “out-of-pocket” costs for those who qualify!
Even better? This “Virtual Care Ecosystem” could potentially provide the U.S. Government with the “silver bullet” needed to reduce healthcare costs in America by up to tens of billions of dollars each year…
Potentially save 100,000 (or more) lives each year…
And potentially offer affordable healthcare for all — or even healthcare at no out-of-pocket cost to patients!
Getting started with Assure Health is simple, easy, and fast.
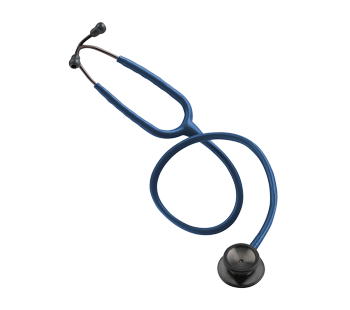
Here’s How It Works…
To get started, a patient fills out the form on the Assure Health website, or calls into their support line. During this process, they collect all the patient’s insurance information to determine eligibility. Assure Health provides total price transparency and lets prospective patients know if they qualify for no out of pocket cost or what their financial obligation will be prior to the first visit.
Next, the patient is onboarded into the ecosystem with a 15-30 minute telemedicine consultation. On this call, one of Assure Health’s licensed doctors will go through the patient’s medical history, prescriptions, and a series of questions to assess the patient’s health and put together a personalized plan to help monitor and improve the patient’s health.
Using their medical judgment, the doctors will determine whether a patient qualifies for remote monitoring and if so, which devices should be ordered for the patient based on their condition and unique health needs.
This usually happens within 48 hours of signing up with Assure Health, but can be scheduled out as far as two weeks depending on the patient’s availability.
After the patient’s virtual onboarding appointment, the appropriate device(s) are shipped out, and will arrive on the patient’s doorstep within 48 hours.
After the patient receives the device(s), they will be assigned a personal care manager — a nurse practitioner — who will be monitoring their condition every day, and will be their dedicated touchpoint going forward.
The best part about Assure Health’s technology?
The patient doesn’t have to manually record – or report – any of their vital signs or biomarkers. All of it is “automatically” collected – and then transmitted – to the patient’s Assure Health provider.
The Math Behind Unicorn MedTech’s
Public multiples in The telemedicine and connected device space currently trade between 30-60 revenue multiples.



If Assure Health maintains an average of $130 per month in revenue per patient and obtains 20,000 patients * $130/month = $31.2 million per year in annual revenue. At a 32x multiple, Assure Health would be valued at approximately $1bn dollars. Of course, no assurance can be given that Assure Health will be able to achieve these milestones.
[Note: This is not a projection or claim of future valuation of Assure Health, only a hypothetical representation of potential value based on existing market comps and national Medicare reimbursement rates. The fair market value – or given multiples of revenue – of any company in this sector could materially change if these reimbursement rates, or other market conditions, change significantly.]
The Math Behind Unicorn MedTech’s
Public multiples in The telemedicine and connected device space currently trade between 30-60 revenue multiples.




If Assure Health maintains an average of $130 per month in revenue per patient and obtains 20,000 patients * $130/month = $31.2 million per year in annual revenue. At a 32x multiple, Assure Health would be valued at approximately $1bn dollars. Of course, no assurance can be given that Assure Health will be able to achieve these milestones.
[Note: This is not a projection or claim of future valuation of Assure Health, only a hypothetical representation of potential value based on existing market comps and national Medicare reimbursement rates. The fair market value – or given multiples of revenue – of any company in this sector could materially change if these reimbursement rates, or other market conditions, change significantly.]
Where American citizens are fully connected with their healthcare provider without stepping foot in a physician’s office every time they need care…
Where doctors and other clinicians can finally provide the level of holistic care to their patients they want to give, but can’t due to factors outside of their control…
Where our citizens can live longer, healthier, and happier lives because their chronic conditions can be better managed.
This future isn’t science fiction.
Thanks to Assure Health’s Virtual Care Ecosystem, this future is happening right now…
And you have an opportunity to help tens of millions of “at-risk” Americans get access to this Virtual Care Ecosystem.
Here Are 9 Reasons To Consider Investing In Assure Health
9 Reasons To Consider Investing In Assure Health
At public market multiples, if Assure Health obtains 20,000 patients for its service, it could be worth $1 billion assuming a 32x multiple of projected annual revenue.
Unlike other expensive therapies and medical devices, as long as the user qualifies for Medicare – and they have qualifying supplemental insurance – they can have access to round-the-clock medical monitoring services, at no out-of-pocket costs, provided that such services are medically necessary given their unique health situation.
The biggest problem with other preventive medicine solutions? Getting the patient to consistently record data AND accurately submit information to their physician.
With this solution, all data is recorded and reported automatically, to any healthcare provider the patient wants to share records with, without the patient having to manually transfer data themselves.
All of the data recorded can be shared with the patients’ physicians and primary care providers. Assure Health has a collaborative approach that aims to give “superpowers” to patients’ primary care provider (PCP) and existing medical teams to deliver the best possible care.
This approach provides what’s known as “continuity of care,” as all electronic health records can be accessed by the patient’s entire network of healthcare providers with the patient’s permission, without the need to constantly restate information.
As a result of this information sharing feature of Assure Health’s platform, every healthcare professional the patient sees can have access to all of the current and relevant information (which in turn helps them improve patient outcomes).
At the time of publishing, we are not aware of any company that is competing with Assure Health’s direct-to-consumer, Medicare-credentialed business model. Assure Health has a clear head start against all other companies in the market.
Assure Health does not manufacture medical devices. Even though Assure Health’s patients utilize FDA approved medical devices, the company does not manufacture those devices, and is therefore not responsible for undergoing any FDA approval or ongoing FDA compliance.
This isn’t a prototype or an idea. Assure Health’s technology and services are currently in market, being used to treat real patients, and the company is receiving recurring revenue.
According to the Centers for Disease Control and Prevention (CDC), each year nearly 900,000 Americans die prematurely from the five leading causes of death: heart disease, cancer, chronic lower respiratory diseases, stroke, and unintentional injuries. However 20 percent to 40 percent of the deaths from each cause could be potentially be prevented.
Assure Health’s “Virtual Care Ecosystem” is designed to more effectively monitor and manage the chronic conditions that often lead to these preventable deaths.
There’s never been a better time than right now to be in Virtual Medicine. Thanks to COVID-19, we’ve seen massive adoption rates from seniors. Now, all they need is a breakthrough product.
Why Now Is The Time to Fight Chronic Disease in America…
For the past 40 years, there’s been a startling trend in the world of healthcare in America.
A massive increase in the number of preventable deaths, in large part due to chronic diseases…
Which are defined by the Centers for Disease Control (CDC) as “conditions that last 1 year or more and require ongoing medical attention or limit activities of daily living or both.”
According to the CDC, six in ten adults in America have some form of chronic disease, and four in ten adults have two or more chronic conditions.
When we look at the Medicare population, these numbers get even more dramatic: Data from the Centers for Medicare and Medicaid Services (CMS) show that over two thirds of Medicare beneficiaries have two or more chronic conditions.
It’s the leading cause of death and disability, as well as the leading driver of the nation’s $3.7 trillion in annual health care costs.
This is equivalent to 19.6 percent of the U.S. GDP in 2016—in other words, nearly one-fifth of the U.S. economy…
And the problem is only getting worse!
The Number of People with Chronic Conditions
is Rapidly Increasing:
According to the Partnership to Fight Chronic Disease…
The most disturbing part of this trend? As people age, the risk of chronic disease increases.
With 10,000 people turning 65 each day, so does the number of people with chronic conditions on Medicare.
According to The Alliance for Aging Research – the nation’s leading non-profit organization dedicated to supporting and accelerating the pace of medical discoveries to improve the universal human experience of aging and health…
99% of Medicare spending is on behalf of beneficiaries with at least one chronic condition…
And the more chronic conditions they have, the more expensive they are to care for.
According to the RAND Corporation’s study, “Multiple Chronic Conditions in the United States”…
Those with five or more chronic conditions spend twice as much on average as those with three or four conditions…
And a whopping 14 times more than people with no chronic conditions!
And this is a huge problem considering…
Drug Costs Are Skyrocketing
In healthcare, there is a strange paradox when you consider the impact of Moore’s Law in the technology sector…
In 1965, Gordon Moore – the CEO and co-founder of Intel – predicted the number of transistors on microchips would double every two years.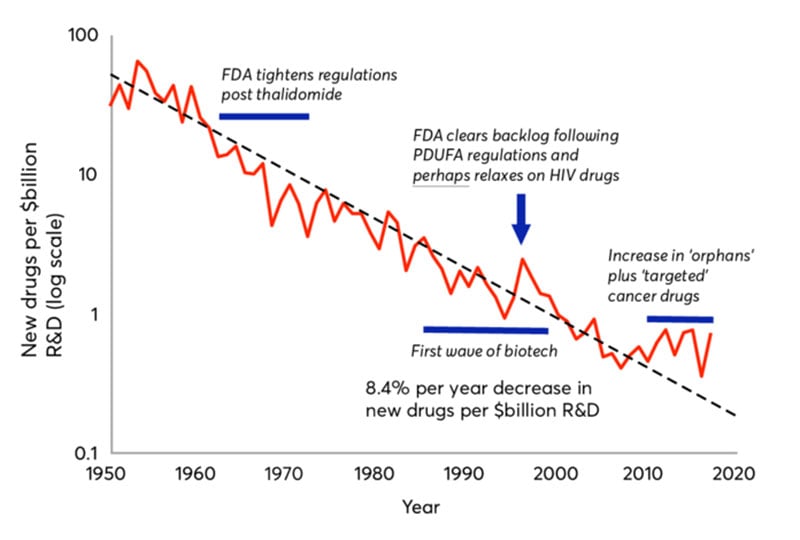
However, in medicine, the opposite has taken place.
According to a 2012 study released by Nature Reviews Drug Discovery…
“The past 60 years have seen huge advances in many of the scientific, technological and managerial factors that should tend to raise the efficiency of commercial drug research and development (R&D).
Yet the number of new drugs approved per billion US dollars spent on R&D has halved roughly every 9 years since 1950, falling around 80-fold in inflation-adjusted terms.”
It’s called “Eroom’s Law” (which is Moore’s Law, but backwards).
To make matters worse, the high costs associated with the higher number of prescriptions can lead to unfortunate results for patients…
In order to reduce costs, they won’t follow their doctor prescribed regimen (called “non-adherence”), which often worsens health outcomes and increases the likelihood of additional – and expensive – hospitalization.
If this trend continues, it likely means more people will be on more medication, at higher costs, for longer.
And the economic toll it’s taking on this country is devastating.
According to the 2020 Report of the Medicare Trustees, published on April 22, 2020…
Under the intermediate assumptions, the assets of the HI trust fund would steadily decrease as a percentage of annual expenditures throughout the short-range projection period, as illustrated in figure II.E1. The ratio declines until the fund is depleted in 2026, the same date as projected last year.
And according to the American Action Forum…
While the bankruptcy projection may snag the headlines, there are three key budgetary numbers that shouldn’t go unnoticed.
To avoid sounding alarmist, the Medicare Board of Trustees has been projecting insolvency dates since 1970, and we’ve been able to continue to push the projected insolvency date…
However, the implications are clear. This situation is not sustainable.

According to the Cato Institute…
As Medicare grows relative to GDP, it will necessarily create some combination of crowding out of other government expenditures, rising taxes, and increasing debt.
At some point higher taxes will slow the economy and more debt will lead to higher interest rates, resulting in a vicious cycle of slower economic growth, exploding government debt, and perhaps even government default.

As Medicare grows relative to GDP, it will necessarily create some combination of crowding out of other government expenditures, rising taxes, and increasing debt.
At some point higher taxes will slow the economy and more debt will lead to higher interest rates, resulting in a vicious cycle of slower economic growth, exploding government debt, and perhaps even government default.
If we don’t do something to get control of chronic disease related expenses, it will not only speed up the likely chance of the Medicare Trust being depleted…
But will continue to deepen the already massive Federal Deficit.
However, Medicare is a “sacred cow” in America. Making budget cuts – or reducing coverage – would be potentially devastating for the tens of millions of people who rely on Medicare for their healthcare.
This means the only plausible option for politicians – and America – to address this crisis?
We must innovate!
And now, with “universal healthcare” becoming a political goal of ever-increasing popularity…
How could politicians deliver this long-standing dream — healthcare for all … without further exploding the swelling federal deficit?
The answer could fit in the palm of your hand, or on the back of your wrist…
Wirelessly transmitting all of your vitals and a whole host of physiologic parameters – straight to a team of qualified doctors and nurse practitioners – who monitor you (or your loved ones) on an ongoing basis.
Thanks to Assure Health, this technology is available right now…
How Preventive Medicine Could Save 100,000’s of Lives – and Hundreds of Billions of Dollars – Each Year
While you might not see splashy headlines about “explosive gains” in the preventive medicine sector, the core thesis is sound and obvious.
As the saying goes, “An ounce of prevention beats a pound of cure.”
And this logical idea has been gaining serious bi-partisan traction over the past decade.
On July 14, 2010, the Center for Medicare & Medicaid Services released a statement stating…

“Today, the Departments of Health and Human Services, Labor, and the Treasury issued new regulations requiring private health plans to cover evidence-based preventive services and to eliminate cost-sharing for preventive care.”
Since then, we’ve seen a flurry of new laws passed to help support the advancement of the cause.
As a part of the American Recovery and Reinvestment Act, all public and private healthcare providers and other eligible professionals (EP) were required to adopt and demonstrate “meaningful use” of electronic medical records (EMR) by January 1, 2014 in order to maintain their existing Medicaid and Medicare reimbursement levels.
Since that date, the use of electronic medical and health records has spread worldwide and shown its many benefits to health organizations everywhere.
Enacted as part of the American Recovery and Reinvestment Act of 2009, the HITECH Act was signed into law on February 17, 2009, to promote the adoption and meaningful use of health information technology.
Before the HITECH Act was passed into law, only 10 percent of hospitals in 2008 had switched from paper files to EHRs. The primary reason why so few healthcare organizations were using electronic records was due to the high expense of changing over. Once the act was passed, the included incentives encouraged healthcare organizations and providers to make the switch to electronic health records.

Signed into law by President Barack Obama on March 23, 2010, the act mandated the inclusion of preventive healthcare – like immunizations, mammograms, and wellness visits – by the insurance providers at no added cost.
Obamacare’s free preventive services help to put the focus on wellness, early detection, and prevention, instead of treatments and cures.
[Note: “Obamacare” did not include any specific provisions for RPM]

EXPANSION OF TELEHEALTH WITH 1135 WAIVER: Under this new waiver, Medicare can pay for office, hospital, and other visits furnished via telehealth across the country and including in patient’s places of residence starting March 6, 2020.
Medicare beneficiaries will be able to receive a specific set of services through telehealth including evaluation and management visits (common office visits), mental health counseling and preventive health screenings.
This will help ensure Medicare beneficiaries, who are at a higher risk for COVID-19, are able to visit with their doctor from their home, without having to go to a doctor’s office or hospital which puts themselves and others at risk.
There are three main types of virtual services physicians and other professionals can provide to Medicare beneficiaries: Medicare telehealth visits, virtual check-ins and e-visits.

On Dec 01, 2020, CMS released a press release stating…
“This final rule delivers on the President’s recent Executive Order on Improving Rural Health and Telehealth Access by adding more than 60 services to the Medicare telehealth list that will continue to be covered beyond the end of the public health crisis (PHE), and we will continue to gather more data and evaluate whether more services should be added in the future.”
On Dec 01, 2020, CMS released a press release stating…
“This final rule delivers on the President’s recent Executive Order on Improving Rural Health and Telehealth Access by adding more than 60 services to the Medicare telehealth list that will continue to be covered beyond the end of the public health crisis (PHE), and we will continue to gather more data and evaluate whether more services should be added in the future.”
The global preventive healthcare technologies and services market size is expected to reach $432.4 billion by 2024.

In response to the COVID-19 crisis, we’ve seen a massive adoption of both telehealth and remote patient monitoring technologies.

There were 3 primary federal stimulus packages addressing the COVID-19 pandemic enacted in March 2020
The CPRSA was an $8.3 billion emergency funding bill that included $500 million to expand Medicare telehealth coverage during emergencies.
The FFCR Act was a relief package focused on expanding COVID-19 testing, supporting Medicaid, and enhancing unemployment benefits. It included a technical change to the CPRSA to further expand Medicare beneficiaries’ telehealth access.
The CARES Act was a sweeping $2.2 trillion economic stimulus package that provided a variety of direct economic support measures. It further expanded coverage and loosened the definitions of Medicare telehealth services.
In addition, CMS issued clarifications further detailing the regulatory waivers and rules. These clarifications, in concert with the emergency declarations and stimulus packages, effectively unshackled telemedicine, resulting in its rapid adoption through the following features.
In April, 2020, Humana had more than 1 million telehealth visits, a daily average of more than 33,000 visits, among its network providers, compared with just a few hundred per day as recently as February, said Dave Icke, vice president of digital health and analytics product for Humana.
According to a survey conducted by Doctor.com in June of 2020:
According to a study conducted by Spyglass Consulting…

According to Grand View Research
In response to the COVID-19 crisis, we’ve seen a massive adoption of both telehealth and remote patient monitoring technologies.

According to Journal of the American Medical Association…
There were 3 primary federal stimulus packages addressing the COVID-19 pandemic enacted in March 2020
The CPRSA was an $8.3 billion emergency funding bill that included $500 million to expand Medicare telehealth coverage during emergencies.
The FFCR Act was a relief package focused on expanding COVID-19 testing, supporting Medicaid, and enhancing unemployment benefits. It included a technical change to the CPRSA to further expand Medicare beneficiaries’ telehealth access.
The CARES Act was a sweeping $2.2 trillion economic stimulus package that provided a variety of direct economic support measures. It further expanded coverage and loosened the definitions of Medicare telehealth services.
In addition, CMS issued clarifications further detailing the regulatory waivers and rules. These clarifications, in concert with the emergency declarations and stimulus packages, effectively unshackled telemedicine, resulting in its rapid adoption through the following features.
In April, 2020, Humana had more than 1 million telehealth visits, a daily average of more than 33,000 visits, among its network providers, compared with just a few hundred per day as recently as February, said Dave Icke, vice president of digital health and analytics product for Humana.
According to a survey conducted by Doctor.com in June of 2020:

According to a study conducted by Spyglass Consulting…
And no surprise, 2020 saw record levels of deal activity in the telemedicine and RPM space.
Notable M&A transactions in 2020:
Not to mention the telehealth company Amwell, who raised $742 million during its 2020 IPO.
However, large funding rounds and splashy exits don’t necessarily translate to better patient outcomes at lower prices.
While most people may be familiar with wearable devices – like Fitbit and Apple Watch – and other virtual medicine providers – like Teladoc…
It’s going to take more than a new software application or a wearable device to solve this growing crisis.

5 Major Challenges That Must Be Addressed to Unlock This Opportunity
One of the biggest challenges for patients with chronic conditions? Following complex and extensive treatment regimens.
As stated earlier, one of the largest drivers of healthcare costs is hospital readmissions; patients with chronic conditions make up a majority of cases.
What drives readmission rates? According to the American Council on Science and Health…
At first glance, it’s easy to blame the hospital or care facility for the problem. However, the truth is always more nuanced.
As mentioned earlier, the more chronic conditions a patient has, the more prescription medicines they have. With more costly – and more complex – treatment plans, it becomes harder and harder to adhere to “doctors’ orders.”

A recent systematic review of peer-reviewed adherence studies finds a median estimate of the cost burden of poor adherence to chronic disease medications is approximately $17,000 per person, per year, (in 2015 dollars).
Updated estimates of the overall burden of suboptimal medication use exceed $500 billion per year in the U.S.
To make matters worse, many patients with chronic conditions have physical challenges that make it hard to get out of bed, let alone travel for regular doctor visits.
This can lead to a vicious cycle of hospitalization, readmission, and additional treatments… both at a great cost to the patients’ health and finances.
The other major challenge for patients with chronic illness is what’s known as continuity of care: do all of the physicians treating the patient know what each other is doing?
If they don’t, it often means the patient receives conflicting advice from each of their healthcare professionals, and are potentially being over-prescribed medication they may or may not need.
This problem is only made worse in rural areas where doctor and nurse turnover rates are the highest, and medical records aren’t kept up to date across all physicians.
Primary care providers are often forced to make treatment and medication decisions based only on a very small sample of imperfect data points.
For example, if a patient has her blood pressure taken three times a year by her primary care provider, the patient’s medication regimen will be based on those numbers, and usually those numbers alone.
“As a doctor sometimes I only see patients two or three times a year, and they’re on blood pressure medications. I only get that one chance in the office, as I’m seeing a patient, to gather up their blood pressure.
So as a doctor, I’m making decisions that are going to impact them for a lifetime, that are going to impact them for a year on one blood pressure reading. That’s just a very simple example, but that is the reality.”
-Dr. Micahel Hafran

First, those numbers are often incorrect as a result of something called White Coat Syndrome: patients’ naturally elevated blood pressure when they go to a doctor’s office.
Second, those numbers represent just a small snapshot in time that is not necessarily representative of a patient’s daily life.
When seniors – especially those with chronic conditions – are treated only for acute issues and are deprived of meaningful, preventive treatment… health outcomes are worse and healthcare costs are dramatically higher.
As patients become more aware of – and engaged in – their own health, they are actively seeking ways to track their most important biomarkers.
However, the real challenge lies in what’s known as clinical integrity: What happens to the data? How is it acted upon? Who is handling the data? How are escalations and interventions handled?
According to the Assure Health team:
“Most companies are unable to answer these basic questions, belying the hollow nature of their remote patient monitoring programs.”
Speaking of remote patient monitoring programs…
Virtual Care technology has been available for several years now.
However, the paradox of these technologies is this: The population that actually needs telehealth and remote patient monitoring services the most, usually have the least access to the technology.
For the majority of Americans, telehealth is a way to get healthcare in a way that is significantly more intimate, quick, and convenient manner.
In practice, this typically means the primary focus of many telehealth services is approaching larger companies and getting them to offer these devices to patients as a benefit of employment…
Generally speaking, that means means younger, healthy people with financial means.
As a result, many “digital health” companies are usually more transaction focused, with the goal of optimizing for volume – not to create a longer term, relationship driven, preventive care solution for the management of chronic conditions.
This issue is exacerbated for people located in rural areas with limited access to remote care technology.
Especially since the challenges with getting rural adoption comes from a sad and unavoidable economic truth…
Rural areas are often more than 100 miles away from a major medical facility with this technology in-place. However, for the majority of physician-owned medical practices that are closer proximity, bearing the financial burden for upgrading their systems is difficult.
Running a successful remote patient monitoring (RPM) program requires the average medical practice to change the way its clinicians and staff deliver patient care. It requires a substantial expansion of responsibilities, such as constant monitoring, support, and monthly reviews of the data.
As a result, the overwhelming majority of primary care providers (PCPs) do not offer RPM as an option to patients.
If patients want to use RPM technologies to take a more active role in their health, their PCP or specialist must already be participating in an RPM program, which is rare.
According to an interview with Roy Schoenberg, CEO of telehealth company Amwell…
The truth is that with these technologies, like any technology, things start very expensive, and then they go down the price chain and they become more and more available to the public.
When it comes down to smaller and smaller physician organizations and groups, these technologies, especially at the level that I just discussed, become cost prohibitive.

In short, there is a tremendous access problem for the patients – and in turn, physicians’ offices – who could benefit most.
This is only exacerbated in the case of the most vulnerable patient populations, who may be unable to leave their homes on a regular basis, and those patients located in rural areas or areas without dense networks of healthcare providers.
This burden is only magnified by a simple fact about Medicare…
In order for physicians to be reimbursed for providing preventive care, they need new “billing codes” to submit to Medicare.
Most doctors are paid the same, regardless of whether you’re sick or healthy. It’s all determined by the billable codes.
Until more meaningful billing codes can be established – especially billing codes that are time based versus flat fee – the risk is often times too great for practices in rural areas to adopt the technology.
This problem is only made worse by the true technological barrier that stands in the way of mass adoption…
According to Jackson Williams, the director of regulatory affairs at Dialysis Patient Citizens, and former health services researcher in the AARP Public Policy Institute…
“The biggest problem confronting Medicare was the inability of its fee-for-service program to address chronic disease care.”
Williams suggests that in order to scale up care coordination for chronic diseases, an old paradigm of thinking must be re-examined: The primary care provider as quarterback.
The current predominant payment model is based on the idea of the primary care physician as “quarterback” of a case management team.
This means the patient’s access to care coordination is dependent on who is “in network.”
This is the opposite of patient-centered; it is 100 percent physician-centric.
That’s why in order to make a real and substantial impact on the chronic disease crisis in America, we have to re-imagine the way we deliver preventive care.
At a macro level, the healthcare system is focused on acute management and not preventive medicine. This traditional model treats patients on a “revolving door” basis.
The patient is seen in an office visit, then follow-up appointments are scheduled at arbitrary time intervals.
Between those scheduled visits, the patient commonly ends up in emergency rooms, hospitals or urgent care centers due to acute flare-ups.
The arrangement is fundamentally grounded in inefficiency, both economically and materially.
The end result?
According to the Annals of Family Medicine…
Many Americans are not receiving recommended health care services. Despite the existence of established clinical guidelines, which are expected to facilitate more consistent and effective medical practice and improve health outcomes, Americans receive only about one half of the applicable services for acute, preventive, and chronic disease care.
INCUMBENT PLAYERS WON’T SOLVE THIS PROBLEM…
For too long, preventive care technologies have remained just out of reach for those populations that need them most.
Current RPM companies take a B2B SaaS approach and license their hardware and software to doctors’ offices and clinics, which are then responsible for developing and administering the program.
However, most of those doctors aren’t equipped to take on the responsibility of running a successful RPM program.
They would have to hire more staff, take significant financial risk, and ensure patients adhere to the program.

Instead, it’s more likely they’ll wait for a smaller startup to take the risk of creating a new ecosystem, and then partner with them once the business model has been proven.
These other companies tend to focus on getting data — vital signs, biomarkers, and various physiologic parameters (like blood pressure, blood sugar, weight, and heart rate) transmitted wirelessly from a patient to a medical professional. Assure Health goes much further, and they go far beyond typical RPM.
They answer the most important question: “Once we have the data, what do we do with it? How do we act on it to really improve patients’ health and lives, and to intervene when necessary?”
According to a 2019 report from McKinsey & Company…
Building a digital health ecosystem can drive tremendous value in the time of disruption.
These ecosystems enable a range of consumer centric services by establishing a network of digital service providers.
If all ecosystem participants could gain access to longitudinal data from payers, providers, social networks, fitness devices, and nutrition apps, they would be better able to develop innovative solutions targeted to individuals and groups.
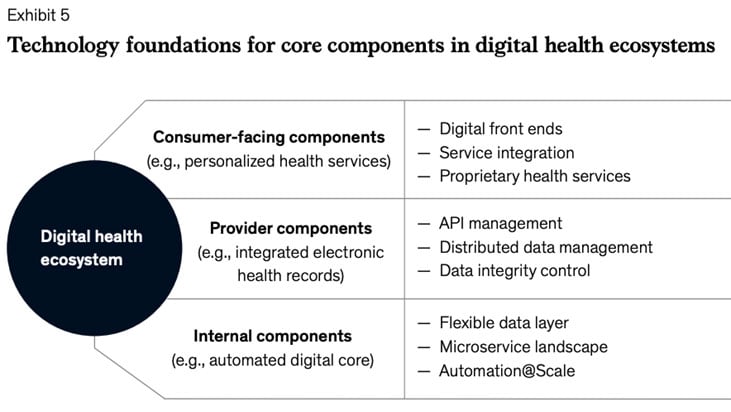
That’s why Assure Health has gone beyond the all-too-common model of creating new apps and tech gadgets…
And instead, are focused on true market innovation.
That’s why they’ve focused on building a truly innovative digital health ecosystem – designed with clinical integrity – to address the most significant problem in America today.

Introducing: “The Assure Health Virtual Care Platform”
To truly understand the opportunity – and why an ecosystem, a full-featured platform, rather than just a single product or service offering, has the greatest potential to solve all of the core challenges in healthcare…
First, a quick primer on how ecosystems work (and what makes them so valuable).
First, they allow horizontal consolidation: multiple providers can consolidate their customer base into a single platform.
Second, they allow for vertical consolidation: the entire customer journey can be delivered in one seamless experience, without ever needing to search outside the ecosystem for needed solutions.
Of course, ecosystem participants don’t try to do this by building everything they need in-house.
Instead, ecosystem organizers create “win-win” partnerships with providers.
This, in turn, drives a profound network effect; By offering products and services that individual companies could not create on their own, ecosystems draw in more and more customers, which creates even more data, which allows artificial intelligence (AI) to fashion even better offerings, which in turn further improves processes and wins more customers.
Along the way, customers’ costs go down even as they gain new experiences, all of which creates new demand for new solutions that are created through data.
That’s exactly the approach Assure Health is taking as part of their ecosystem building strategy.
According to the founders…
We have created a legally-compliant, direct-to-consumer RPM program, which, in truth, goes far beyond what most people ever contemplated when RPM was devised — providing a level of high-touch remote healthcare that has historically been incredibly challenging, if not impossible, to deliver .
We are able to market and offer our program directly to consumers, without their having to switch doctors.
We have built an entire clinical infrastructure to support this, so we can offer world-class care in collaboration with their existing doctors.
And for those with qualifying coverage, we can do all of this at a $0 out-of-pocket cost.
The value we bring to the ecosystem is based on two core functions.
First, we’ve developed a purpose-built – and scalable – clinical infrastructure that solves a lot of the major problems preventing widespread adoption.
Second, we’re positioned to assume the role of “quarterback” and become the most frequent touch point in the patient experience.
This, in turn, provides all of our ecosystem participants the opportunity to focus on improving patient outcomes… NOT dealing endlessly with compliance, regulatory burdens, and administrative minutiae.
To participate successfully in ecosystems, traditional companies must often change the way they think about customers.
Instead of limiting themselves to services within their historical industry borders, they may venture beyond in an effort to serve customers from one end of the customer journey to the other.
Unlike other telehealth and RPM solutions, the Assure Health Virtual Care Platform is – at the time of publishing – the only ecosystem-based solution that has the potential to solve many of the major challenges in preventive care.
Assure health Solution #1:
As mentioned earlier, adherence is one of the most significant problems for patients with chronic conditions.
Why? Because it’s almost impossible to know – with certainty – if the patient is following the prescribed treatment.
Currently, the only measure of adherence most physicians have is whether or not a prescription was filled. However, this doesn’t mean the patient is taking their medication (or doing so correctly).
Taking Stock: Patient Medication Adherence and Chronic Disease Management: A NEHI Policy Brief
Studies of medication adherence generally track fill and refill data to delineate whether a patient picks up a medication once it is prescribed (primary adherence), and whether a patient fills and refills a prescription in keeping with the prescriber’s instructions (secondary adherence.)
Thanks to Assure Health’s Virtual Care Ecosystem, patients’ vitals are monitored – and transmitted – in near-real time… without the patient having to manually transfer data themselves.
Assure Health prepares and pre-provisions each device before shipping to patients so everything works right out of the box. There are no apps to download and no complicated technology to learn how to use.
All of the devices used on the Assure Health Ecosystem include embedded cellular modems. This means data is automatically transmitted securely into compliant electronic health records (EHR)…
It’s a frictionless data collection process that presents a holistic picture of the patient by having true, everyday measurements.
This creates the opportunity for the patients’ care providers to see far more accurate data regarding adherence rates.
According to Assure Health’s management team…
“We are closer than almost anyone to having the highest fidelity data related to adherence because we actually see their vitals and have a constant stream of physiologic parameters coming into our clinicians.
Because we validate and collect large amounts of data in real time, we are providing efficacy information. It’s almost like we are running a clinical trial of one.”
Continuous measurement of the patient’s medication provides transparency into three essential elements of medication use: initiation of treatment, adherent execution, and persistent use for the entire duration of treatment.
This, in turn, allows Assure Health clinicians to step in and provide meaningful interventions that can improve patient outcomes… with the potential to lower the overall costs of care by reducing (or preventing) hospital readmission.
To be clear, data collection alone isn’t enough to deliver a meaningful impact on patient outcomes.
A lot of companies have the gadgets and they have the data… but the really difficult part that historically hasn’t been solved is analyzing the data and making clinically meaningful decisions.
You could argue that data without answering that question is maybe even worse than no data at all — a false sense of security.
How does the data get interpreted? How do interventions happen? How do we use the data to deliver real results?
These are some of the questions that Assure Health’s approach answers.
Assure health Solution #2:
With Assure Health, patients – and their families – get a second set of well-trained eyes (a physician or nurse practitioner) reviewing their numbers every single day.
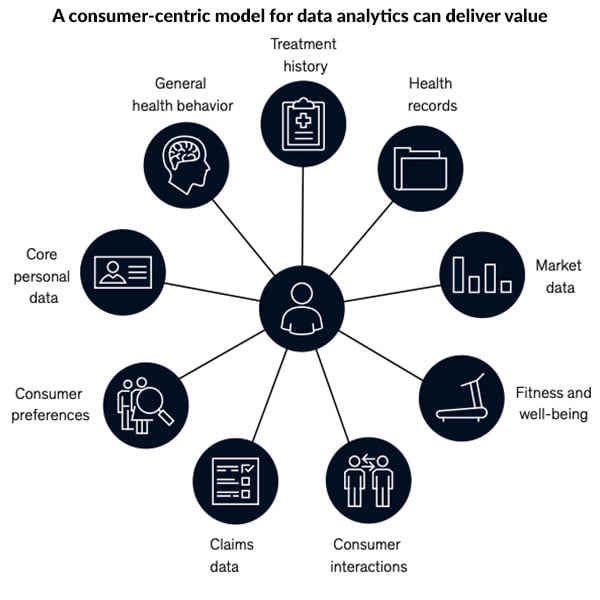
They get the knowledge that they are using a concierge medicine-style early warning system that can catch issues before they become major… help to eliminate avoidable hospitalizations…and work towards improving their overall health.
And they get a personal care manager (who is a licenced nurse practitioner) to have calls with them throughout the month, review their health, and keep them safe and healthy.
According to Assure Health’s management team…
“Once we have a patient, we often become the most frequent and trusted healthcare touchpoint the patient has. No other provider is working with them every day.”
This, in turn, supports the mandate of the American Recovery and Reinvestment Act, which requires all public healthcare providers to show “Meaningful use” of electronic health records.
“Meaningful use” of electronic health records (EHR), as defined by HealthIT.gov, consists of using digital medical and health records to achieve the following:
Additionally, all of this data can be shared with the patients’ primary care providers, as well as all other physicians they see.
“Primary care doctors love working with us because we close the gaps. We make sure that they have access to a patient’s data, their vital signs, their information, with a much higher degree of frequency than they’ve ever had before. And we supply them with this information in advance of any routine doctor’s appointments so that they have the superpowers of having visibility into patients’ health lives on a daily basis.”
– Jeff Nadel, Co-Founder of Assure Health

Because there is a single source of truth for all of their vitals, this creates an opportunity for all of the patients’ care to be properly coordinated and work towards better healthcare outcomes.
Assure health Solution #3:
Perhaps the single most obvious advantage of Assure Health’s ecosystem is the out-of-pocket cost to the patient.
For any patient on Medicare who qualifies and for whom Assure Health’s services are medically necessary, 80% of all costs would be covered, with only 20% owed by the patient. However, if the patient also has supplemental medical coverage, often known as Medigap or Medicare Supplement plans – which 32 million Medicare patients do – it requires zero out of pocket costs, exclusive of any applicable deductibles.
At this point, the only barrier to adoption is a lack of awareness: Most people on Medicare have no idea they qualify for this program, and they don’t know where to turn to get this level of care.
That’s why Assure Health is currently seeking to raise capital via crowdfunding; they can both raise funds and drive awareness at the same time.
Assure health Solution #4:
Unlike other telehealth companies, Assure Health insists on using only licensed medical professionals who are specially trained in delivering remote care services and who are diligently screened for the best possible “digital bedside manner.”
Their goal? Provide patients the best healthcare experience they’ve ever had!
All clinicians rendering services are specially trained and experienced not only in rendering care remotely, but also in the specifics of monitoring physiologic parameters on a regular basis and communicating with patients accordingly.
But perhaps the most significant impact of Assure Health? It helps physicians spend more time with patients and deliver more meaningful care.
The same can’t be said about companies like Teladoc or Amwell, where physicians see different patients every day on a more transactional basis.
With Assure Health, it’s all relationship based. Physicians have a greater opportunity to make a real impact on patient outcomes.
According to Annie Muehlberger, a Nurse Practitioner and personal care manager with Assure Health:

“Assure Health brings a personal aspect to telemedicine because at every visit or every phone call, text message, you will be getting the same person every time.
You will not have your information passed off from one care member to another. You will have the same care team member at every time as soon as you are introduced to them. And you get to know them.
They get to know your family, you get to know theirs and at all times you get this bond and trust. And it’s more personalized that you’re not expecting a different person every time or you have to explain your situation at every phone call. You just know that the other person at the end of the line knows your situation.
As a nurse practitioner who has worked in other practices, I have to say, this is among the most rewarding work I’ve ever done.“

You will not have your information passed off from one care member to another. You will have the same care team member at every time as soon as you are introduced to them. And you get to know them.
They get to know your family, you get to know theirs and at all times you get this bond and trust. And it’s more personalized that you’re not expecting a different person every time or you have to explain your situation at every phone call. You just know that the other person at the end of the line knows your situation.
As a nurse practitioner who has worked in other practices, I have to say, this is among the most rewarding work I’ve ever done.“
Furthermore, Assure Health has already developed algorithms to help clinicians guide their decision making, and eliminate the annoying grunt work that is unfulfilling.
Instead of trying to automate clinicians out of a job, Assure Health is staking their future on using technology to allow clinicians to focus on building a deeply personal relationship with the patient.
The end result?
Assure health Solution #5:
Assure Health’s Virtual Care Ecosystem is solving a massive problem; both at the level of the individual patient… and at a macro/societal level by addressing a healthcare system overburdened with costs stemming from a lack of preventive medicine.
Assure Health uses the latest technology – and licensed clinicians – to remotely monitor the health of seniors with chronic conditions to keep them healthy and safe.
They’re able to deliver personalized, concierge-level care at little to no out-of-pocket cost to tens of millions of prospective patients.
For patients whose medical conditions warrant Assure Health’s services, this eliminates financial barriers to adoption, thereby dramatically expanding access to millions of people who otherwise may not have the privilege of this level of care.
There is an incredible “stickiness” to the product: For many patients who already take their blood sugar or blood pressure, no behavioral change is required; for those who don’t, they come to rely on the comfort of having a clinician looking over their shoulder every day.
And now, you have the opportunity to be part of their bold vision…

RISK FACTORS
A crowdfunding investment involves risk. You should not invest any funds in this offering unless you can afford to lose your entire investment.
In making an investment decision, investors must rely on their own examination of the issuer and the terms of the offering, including the merits and risks involved. These securities have not been recommended or approved by any federal or state securities commission or regulatory authority. Furthermore, these authorities have not passed upon the accuracy or adequacy of this document.
The U.S. Securities and Exchange Commission does not pass upon the merits of any securities offered or the terms of the offering, nor does it pass upon the accuracy or completeness of any offering document or literature.
These securities are offered under an exemption from registration; however, the U.S. Securities and Exchange Commission has not made an independent determination that these securities are exempt from registration.
1. Discuss the material factors that make an investment in the issuer speculative or risky:
An investment in the Company involves a high degree of risk. You should carefully consider the risks described above and those below before deciding to purchase any securities in this offering. If any of these risks actually occurs, our business, financial condition or results of operations may suffer. As a result, you could lose part or all of your investment.
Risks Related to the Company
We have a limited operating history upon which you can evaluate our performance, and accordingly, our prospects must be considered in light of the risks that any new company encounters.
We were formed under the laws of Wyoming on May 29, 2020 and have since redomiciled under the laws of Delaware. We have limited operations and minimal revenues to date. We are in the development stage, and our future operations are subject to all of the risks inherent in the establishment of a new business enterprise. The likelihood of the success of our company must be considered in light of the problems, expenses, difficulties, complications and delays frequently encountered in connection with the development of a telehealth platform that requires significant scale. There can be no assurance that future revenues will be significant, that we will be profitable or that we will have sufficient funds available to complete our marketing and development programs or to market any new services which we may develop. We currently have operating losses, have no substantive source of operating revenue, are unable to self-finance operations, have limited resources, and there can be no assurance that we will be able to develop such revenue sources or that our operations will become profitable, even if we are able to build brand awareness.
The telehealth market is immature and unpredictable, and if it does not develop, if it develops more slowly than we expect, if it encounters negative publicity or if limitations on reimbursement or difficulties in obtaining regulatory approvals impede our ability to adopt telehealth, the growth of our business will be harmed.
With respect to our telehealth solution, the telehealth market is relatively new and unproven, and it is uncertain whether it will achieve and sustain high levels of demand, consumer acceptance and market adoption. Our success will depend to a substantial extent on the willingness of customers to use our telehealth and remote patient monitoring solution, as well as on our ability to demonstrate the value of our telehealth solution to health plans and other purchasers of healthcare for beneficiaries. Negative publicity concerning our telehealth solution or the telehealth market as a whole could limit market acceptance of our solution. Changes by state professional licensing boards to the standards of care or other requirements governing the practice of telehealth, including any such requirements from federal regulatory bodies, could impact the success of our telehealth solution. Additionally, reimbursement may not be available from government and third-party payors for our current or proposed service offerings. Similarly, individual and healthcare industry concerns or negative publicity regarding patient confidentiality and privacy in the context of telehealth could limit market acceptance of our solution. If any of these events occurs, it could have a material adverse effect on our business, financial condition or results of operations.
In order for the Company to compete and grow, it must attract, recruit, retain and develop the necessary personnel who have the needed experience.
Recruiting and retaining highly qualified personnel is critical to our success. These demands may require us to hire additional personnel and will require our existing management personnel to develop additional expertise. We face intense competition for personnel. The failure to attract and retain personnel or to develop such expertise could delay or halt the development and commercialization of our service offerings. If we experience difficulties in hiring and retaining personnel in key positions, we could suffer from delays in business development, loss of customers and sales and diversion of management resources, which could adversely affect operating results. Our consultants and advisors may be employed by third parties and may have commitments under consulting or advisory contracts with third parties that may limit their availability to us.
Quality management plays an essential role in determining and meeting customer requirements, preventing defects, improving the Company’s services and maintaining the integrity of the data that supports the safety and efficacy of our services.
Our future success depends on our ability to maintain and continuously improve our quality management program. An inability to address a quality or safety issue in an effective and timely manner may also cause negative publicity, a loss of customer confidence in us or our current or future service offerings, which may result in the loss of sales and difficulty in successfully launching new service offerings. In addition, a successful claim brought against us in excess of available insurance or not covered by indemnification agreements, or any claim that results in significant adverse publicity against us, could have an adverse effect on our business and our reputation.
Our telehealth business depends on our ability to maintain and expand a network of qualified physicians and other healthcare providers through affiliated professional entities that Assure Health Corporation does not own. If we are unable to do so, our future growth would be limited and our business, financial condition and results of operations would be adversely affected.
Our success is dependent upon our continued ability to maintain a network of qualified physicians and other healthcare providers, and fulfilling our client service obligations requires we maintain a robust supply of these qualified physicians and other healthcare providers. As described above in the “Governmental/Regulatory Approval and Compliance” section, certain state laws prohibit Assure Health Corporation from employing its own medical providers and from directing the clinical practice of medical providers. Thus, like all other compliant telehealth companies, we will depend on third-party entities not owned or controlled by us to provide us with the qualified healthcare providers we need to deliver quality services to patients. If that entity is unable to recruit and retain board-certified physicians and other healthcare professionals and/or we are unable to maintain our relationship with them, it would have a material adverse effect on our business and ability to grow and would adversely affect our results of operations. Further, in any particular market, these providers and/or entities could demand higher payments or take other actions that could result in higher costs, less attractive service for our clients or difficulty meeting legal, regulatory or accreditation requirements. Our ability to develop and maintain satisfactory relationships with these entities and providers also may be negatively impacted by other factors not associated with us, such as changes in Medicare and/or Medicaid reimbursement levels, other pressures on healthcare providers, and consolidation activity among hospitals, physician groups and healthcare providers. The failure to maintain or to secure new cost-effective relationships through which we can source providers may result in a loss of or inability to grow our client base, higher costs, healthcare provider network disruptions, less attractive service for our clients and/or difficulty in meeting regulatory or accreditation requirements, any of which could have a material adverse effect on our business, financial condition and results of operations.
We may implement new lines of business or offer new products and services within existing lines of business.
There are substantial risks and uncertainties associated with these efforts, particularly in instances where the markets are not fully developed. In developing and marketing new lines of business and/or new products and services, we may invest significant time and resources. Initial timetables for the introduction and development of new lines of business and/or new products or services may not be achieved and price and profitability targets may not prove feasible. We may not be successful in introducing new products and services in response to industry trends or developments in technology, or those new products or services may not achieve market acceptance. As a result, we could lose business, be forced to price products and services on less advantageous terms to retain or attract clients, or be subject to cost increases. As a result, our business, financial condition or results of operations may be adversely affected.
The Company’s success depends on the experience and skill of the board of directors, its executive officers and key employees.
In particular, the Company is dependent on Jeffrey Nadel, who is the CEO and a director of the Company; Craig Bolz, who is the COO and a director of the Company; and Dr. Michael Hafran, who is the Medical Director of the Company. The loss of Jeffrey Nadel, Craig Bolz, Dr. Michael Hafran or any key employees could harm the Company’s business, financial condition, cash flow and results of operations.
If we are unable to protect the confidentiality of our trade secrets, our business and competitive position would be harmed.
We currently rely on trade secrets, including unpatented know-how and other proprietary information, to maintain our competitive position. We seek to protect these trade secrets, in part, by entering into non-disclosure and confidentiality agreements with parties who have access to them, such as our employees, corporate collaborators, outside scientific collaborators, contract manufacturers, consultants, advisors and other third parties. We also seek to enter into confidentiality and invention or patent assignment agreements with our employees and consultants. Despite these efforts, any of these parties may breach the agreements and disclose our proprietary information, including our trade secrets, and we may not be able to obtain adequate remedies for such breaches. Our trade secrets may also be obtained by third parties by other means, such as breaches of our physical or computer security systems. Enforcing a claim that a party illegally disclosed or misappropriated a trade secret is difficult, expensive and time-consuming, and the outcome is unpredictable. In addition, some courts inside and outside the United States are less willing or unwilling to protect trade secrets. If any of our trade secrets were to be lawfully obtained or independently developed by a competitor, we would have no right to prevent them, or those to whom they communicate it, from using that technology or information to compete with us. If any of our trade secrets were to be disclosed to or independently developed by a competitor, our competitive position would be harmed.
We face risks related to the storage of customers’ confidential and proprietary information.
Our Assure Health Platform is being designed to maintain the confidentiality and security of our customers’ confidential and proprietary data stored on our server systems, which may include sensitive personal data. However, any accidental or willful security breaches or other unauthorized access to these data could expose us to liability for the loss of such information, time-consuming and expensive litigation and other possible liabilities as well as negative publicity. Techniques used to obtain unauthorized access or to sabotage systems change frequently and generally are difficult to recognize and react to. We may be unable to anticipate these techniques or implement adequate preventative or reactionary measures.
Software failures, breakdowns in the operations of our servers and communications systems or the failure to implement system enhancements could harm our business.
The operational success of our Assure Health platform will depend on the efficient and uninterrupted operation of our servers and communications systems. A failure of our network or data gathering procedures could impede services and could result in the loss of our customers. Despite any precautions we take, damage from fire, floods, hurricanes, power loss, telecommunications failures, computer viruses, break-ins and similar events at our computer facilities could result in interruptions in the flow of data to our servers and from our servers to our clients. In addition, any failure by our computer environment to provide our required data communications capacity could result in interruptions in our service. In the event of a server failure, we could be required to transfer our client data collection operations to an alternative provider of server hosting services. Such a transfer could result in delays in our ability to deliver our products and services to our clients.
Additionally, significant delays in the planned delivery of system enhancements, improvements and inadequate performance of the systems once they are completed could damage our reputation and harm our business. Long-term disruptions in the infrastructure caused by events such as natural disasters, the outbreak of war, the escalation of hostilities and acts of terrorism, could adversely affect our businesses. Although, we plan to carry insurance for our business operations, our coverage might not be adequate to compensate us for all losses that may occur.
We are subject to income taxes as well as non-income based taxes, such as payroll, sales, use, value-added, net worth, property and goods and services taxes, in the U.S.
Significant judgment is required in determining our provision for income taxes and other tax liabilities. In the ordinary course of our business, there are many transactions and calculations where the ultimate tax determination is uncertain. Although we believe that our tax estimates are reasonable: (i) there is no assurance that the final determination of tax audits or tax disputes will not be different from what is reflected in our income tax provisions, expense amounts for non-income based taxes and accruals and (ii) any material differences could have an adverse effect on our financial position and results of operations in the period or periods for which determination is made.
Successful development of our service offerings is uncertain.
Our development of current and future service offerings are subject to the risks of failure and delay inherent in the development of new business solutions based on new technologies, including failure to achieve market acceptance, and the emergence of superior or equivalent products or business models.
Because of these risks, our research and development efforts may not result in any commercially viable service offerings. If a significant portion of these development efforts are not successfully completed, required regulatory approvals are not obtained, or any approved service offerings are not commercially successfully, our business, financial condition, and results of operations may be materially harmed.
We might incur substantial expense to develop our telehealth and remote patient monitoring platform which may never become sufficiently successful.
Our growth strategy includes the successful launch of our telehealth and remote patient monitoring platform. Although management will take every precaution to ensure that our telehealth and remote patient monitoring platform will, with a high degree of likelihood, achieve commercial success, there can be no assurance that this will be the case. The causes for failure of our platform, once commercialized, can be numerous, including (i) market demand for our platform proves to be smaller than we expect; (ii) our telehealth and remote patient monitoring platform turns out to be uneconomic; and (iii) additional regulatory requirements may increase the overall costs of the development.
Political, economic and regulatory influences are subjecting the healthcare industry to potential fundamental changes that could substantially affect our results of operations.
Government and private sector initiatives to limit the growth of healthcare costs, including price regulation, competitive pricing, coverage and payment policies, comparative effectiveness of therapies, technology assessments and alternative payment models, are continuing. These changes are causing the marketplace to put increased emphasis on the delivery of more cost-effective treatments. Such healthcare reform legislation may materially impact us. Certain provisions of the legislation will not be effective for a number of years and it is unclear what the full impact of the legislation will be. Provisions of this legislation, including Medicare provisions aimed at improving quality and decreasing costs, comparative effectiveness research, an independent payment advisory board, and pilot programs to evaluate alternative payment methodologies, could meaningfully change the way healthcare is developed and delivered, and may adversely affect our business and results of operations. Further, we cannot predict what healthcare programs and regulations will be ultimately implemented at the federal or state level, or the effect of any future legislation or regulation in the U.S. or internationally. However, any changes that lower reimbursements for our services, reduce medical procedure volumes or increase cost containment pressures on us or other participants in the healthcare industry could adversely affect our business and results of operations.
Recent and frequent state legislative and regulatory changes specific to telemedicine may present us with additional requirements and state compliance costs, with potential operational impacts in certain jurisdictions.
In recent years, states have adopted an abundance of new legislation and regulations specific to telemedicine. In some cases, this legislation and regulation, typically targeting “direct to consumer” telehealth service offerings, incorporates informed consent, modality, medical record, and other requirements. Thus, where new legislation and regulations apply to our telemedicine solutions, we may incur costs to monitor, evaluate, and modify operational processes for compliance. All such activities increase our costs and could, in certain circumstances, impact our ability to make available telemedicine services in a particular state.
Products that we source, distribute or market are required to comply with regulatory requirements.
To lawfully operate our businesses, we are required to hold permits, licenses and other regulatory approvals from, and to comply with operating and security standards of, governmental bodies. Failure to maintain or renew necessary permits, licenses or approvals, or noncompliance or concerns over noncompliance may result in suspension of our ability to source and distribute products used in our service offerings or criminal and civil sanctions and could have an adverse effect on our results of operations and financial condition.
The commercial success of our business will depend in part upon the level of reimbursement our affiliated healthcare providers receive from third party payors such as government health administration authorities.
The commercial success of our business will depend, in part, on the extent to which reimbursement for the costs of our services and related products will be available from third-party payors such as government health administration authorities, private health insurers, managed care programs, and other organizations. Adequate third-party insurance coverage may not be available for our customers to accept our price levels. The result of this occurring would be to reduce our revenues from our customers which could have a material adverse effect on our business, financial condition and prospects.
We face significant competition from other telemedicine companies.
Our services and products face unique groupings of competitive technologies depending on the application. Not all competitive technologies and services are relevant in each application and market. We face potential competition from many different sources, including major telemedicine companies, healthcare companies, technology companies and insurance providers.
Many of our competitors may have significantly greater financial resources and expertise in research and development, manufacturing, preclinical testing, conducting clinical trials, obtaining regulatory approvals and marketing approved products than we do. Mergers and acquisitions in the pharmaceutical, biotechnology and diagnostic industries may result in even more resources being concentrated among a smaller number of our competitors. These competitors also compete with us in recruiting and retaining qualified scientific and management personnel and establishing clinical trial sites and patient registration for clinical trials, as well as in acquiring technologies complementary to, or necessary for, our programs. Smaller or early-stage companies may also prove to be significant competitors, particularly through collaborative arrangements with large and established companies.
Our planned manufacturing activity is subject to certain risks.
We may manufacture the products offered to our customers as part of our service offerings in the future. As a result, we may be dependent upon the uninterrupted and efficient operation of our manufacturing facility and our distribution facilities throughout the country. Our manufacturing facilities and distribution facilities may be subject to the risk of catastrophic loss due to, among other things, earthquake, fire, flood, terrorism or other natural or man-made disasters, as well as occurrence of significant equipment failures. If any of these facilities were to experience a catastrophic loss, it would be expected to disrupt our operations and could result in personal injury or property damage, damage relationships with our customers or result in large expenses to repair or replace the facilities or systems, as well as result in other liabilities and adverse impacts.
We may contract with third-party manufacturers to produce certain products in the future in accordance with our specifications and standards. These contract manufacturers are subject to the same risks as our manufacturing facility as noted above. While we plan to implement stringent quality control procedures to verify that our contract manufacturers comply with our specifications and standards, we will not have full control over their manufacturing activities. Any difficulties, delays and defects in product delivery resulting from the activities of our contract manufacturers may have an adverse effect on our business and results of operations.
We are dependent on our collaborative agreements for the development of our Assure Health platform, which exposes us to the risk of reliance on the viability of third parties.
In conducting our research and development activities, we will in the future rely on collaborative agreements with third parties such as manufacturers, contract research organizations, commercial partners and governmental agencies for both strategic and financial resources. The loss of, or failure to perform by us or our partners under, any applicable agreements or arrangements, or our failure to secure additional agreements, would substantially disrupt or delay our research and development and commercialization activities. Any such loss would likely increase our expenses and materially harm our business, financial condition and results of operation.
Reliance on third-party relationships and outsourcing arrangements could adversely affect our business.
We utilize third parties, including suppliers, alliances with other med-tech based companies, and third-party service providers, for the platform development, the manufacture of certain products employed in our service offerings, support for information technology systems, and certain financial transactional processes. Outsourcing these functions involves the risk that the third parties may not perform to our standards or legal requirements, may not produce reliable results, may not perform in a timely manner, may not maintain the confidentiality of our proprietary information, or may fail to perform at all. Failure of these third parties to meet their contractual, regulatory, confidentiality, or other obligations to us could have a material adverse effect on our business.
The forecasts of market growth included in our business plan and investor presentations may prove to be inaccurate, and even if the markets in which we compete achieve the forecasted growth, we cannot assure you our business will grow at similar rates, if at all.
Growth forecasts are subject to significant uncertainty and are based on assumptions and estimates that may not prove to be accurate. The forecasts in our business plan and investor presentations may prove to be inaccurate. Even if these markets experience the forecasted growth described in our business plan, we may not grow our business at similar rates, or at all. Our growth is subject to many factors, including our success in implementing our business strategy, which is subject to many risks and uncertainties. Accordingly, the forecasts of market growth included in our business plan should not be taken as indicative of our future growth.
We will need additional financing to execute our business plan, which we may not be able to secure on acceptable terms, or at all.
We will require additional financing in the near and long term to fully execute our business plan. Our success depends on our ability to raise such additional financing on reasonable terms and on a timely basis. Conditions in the economy and the financial markets may make it more difficult for us to obtain necessary additional capital or financing on acceptable terms, or at all. If we cannot secure sufficient additional financing, we may be forced to forego strategic opportunities or delay, scale back or eliminate further development of our goals and objectives, operations and investments or employ internal cost savings measures.
We plan to obtain insurance that may not provide adequate levels of coverage against claims.
We plan to obtain insurance customary for businesses of our size and type. However, there are types of losses we may incur that cannot be insured against or that we believe are not economically reasonable to insure. Such losses could have a material adverse effect on our business and results of operations.
Risks Related to the Company’s Securities and this Offering
Affiliates of our company, including officers, directors and existing stockholder of our company, may invest in this offering and their funds will be counted toward our achieving the minimum amount.
There is no restriction on our affiliates, including our officers, directors and existing stockholders, investing in the offering. As a result, it is possible that if we have raised some funds, but not reached the minimum amount, affiliates can contribute the balance so that there will be a closing. The minimum amount is typically intended to be a protection for investors and gives investors confidence that other investors, along with them, are sufficiently interested in the offering and our company and its prospects to make an investment of at least the minimum amount. By permitting affiliates to invest in the offering and make up any shortfall between what non-affiliate investors have invested and the minimum amount, this protection is largely eliminated. Investors should be aware that no funds other than their own and those of affiliates investing along with them, may be invested in this offering.
We intend to use some of the proceeds from the offering for unspecified working capital.
This means that we have ultimate discretion to use this portion of the proceeds as we see fit and have chosen not to set forth any specific uses for you to evaluate. The net proceeds from this offering will be used for the purposes, which our management deems to be in our best interests in order to address changed circumstances or opportunities. As a result of the foregoing, our success will be substantially dependent upon our discretion and judgment with respect to application and allocation of the net proceeds of this offering. We may choose to use the proceeds in a manner that you do not agree with and you will have no recourse. A use of proceeds that does not further our business and goals could harm our company and its operations and ultimately cause you to lose all or a portion of your investment.
We are not subject to Sarbanes-Oxley regulations and lack the financial controls and safeguards required of public companies.
We do not have the internal infrastructure necessary, and are not required, to complete an attestation about our financial controls that would be required under Section 404 of the Sarbanes-Oxley Act of 2002. There can be no assurance that there are no significant deficiencies or material weaknesses in the quality of our financial controls. We expect to incur additional expenses and diversion of management’s time if and when it becomes necessary to perform the system and process evaluation, testing and remediation required in order to comply with the management certification and auditor attestation requirements.
The securities being sold in this offering will not be freely tradable until one year from the initial purchase date. Although our securities may be tradable under federal securities law, state securities regulations may apply, and each investor should consult with his or her attorney.
You should be aware of the long-term nature of this investment. There is not now and likely will not be a public market for our securities. Because our securities have not been registered under the Securities Act or under the securities laws of any state or non-United States jurisdiction, our securities have transfer restrictions and cannot be resold in the United States except pursuant to Rule 501 of Regulation CF. It is not currently contemplated that registration under the Securities Act or other securities laws will be effected. Limitations on the transfer of the securities may also adversely affect the price that you might be able to obtain for our securities in a private sale. Investors should be aware of the long-term nature of their investment in the Company. Each investor in this offering will be required to represent that it is purchasing the securities for its own account, for investment purposes and not with a view to resale or distribution thereof.
Neither the offering nor the securities have been registered under federal or state securities laws, leading to an absence of certain regulation applicable to us.
No governmental agency has reviewed or passed upon this offering, our company or any Securities of our company. We also have relied on exemptions from securities registration requirements under applicable state securities laws. Investors, therefore, will not receive any of the benefits that such registration would otherwise provide. Prospective investors must therefore assess the adequacy of disclosure and the fairness of the terms of this offering on their own or in conjunction with their personal advisors.
No Guarantee of Return on Investment
There is no assurance that an investor will realize a return on its investment or that it will not lose its entire investment. For this reason, each investor should read the Form C and all Exhibits carefully and should consult with its own attorney and business advisor prior to making any investment decision.
A majority of our company is owned by a small number of owners.
Prior to the offering, our officers, directors and those of our stockholders who own ten percent or more of our securities collectively own directly or indirectly approximately 81.66% of our company. Subject to any fiduciary duties owed to our other owners or investors under Delaware law in the case of our officers and directors, these stockholders may be able to exercise significant influence over matters requiring owner approval, including the election of directors or managers and approval of significant company transactions, and will have significant control over our management and policies. These control persons may have interests that are different from yours. For example, they may support proposals and actions with which you may disagree. The concentration of ownership could delay or prevent a change in control of our company or otherwise discourage a potential acquirer from attempting to obtain control of the Company, which in turn could reduce the price potential investors are willing to pay for our company. In addition, these control persons could use their voting influence to maintain the Company’s existing management, delay or prevent changes in control of our company, or support or reject other management and board proposals that are subject to owner approval.
We have the right to extend the offering deadline.
We may extend the offering deadline beyond what is currently stated herein. While you have the right to cancel your investment in the event the Company extends the Offering Deadline, if you choose to reconfirm your investment, your investment may continue to be held in escrow while we attempt to raise the minimum amount even after the offering deadline stated in this offering statement is reached. Your investment will not be accruing interest during this time and will simply be held until such time as the new offering deadline is reached without our company receiving the minimum amount, at which time committed funds will become immediately available for withdrawal from the investor’s brokerage account maintained with the Intermediary without interest or deduction, or until we receive the minimum amount, at which time it will be released to us to be used as set forth herein. Upon or shortly after release of such funds to us, the securities will be issued and distributed to you.
Your ownership of the shares will be subject to dilution.
If we conduct subsequent offerings of securities, issue shares pursuant to a compensation or distribution reinvestment plan or otherwise issues additional shares, investors who purchase securities in this offering who do not participate in those other stock issuances will experience dilution in their percentage ownership of our company’s outstanding shares. Furthermore, shareholders may experience a dilution in the value of their underlying shares depending on the terms and pricing of any future share issuances (including the underlying shares being sold in this offering) and the value of our assets at the time of issuance.
Management has discretion over proceeds of this offering.
We expect to use the net proceeds of this offering, over time, for general marketing and advertising, leasing costs, debt repayment and general working capital. However, we have no current specific plans for the net proceeds of this offering other than as outlined in the use of proceeds section of this offering statement. As a result, our management will have the discretion to allocate the net proceeds to uses that investors may not deem desirable. There can be no assurance that the net proceeds can or will be invested to yield a significant return.
The securities will be equity interests in our company and will not constitute indebtedness.
The securities will rank junior to all existing and future indebtedness and other non-equity claims on our company with respect to assets available to satisfy claims on the Company, including in a liquidation of our company. Additionally, unlike indebtedness, for which principal and interest would customarily be payable on specified due dates, there will be no specified payments of dividends with respect to the securities and dividends are payable only if, when and as authorized and declared by us and depend on, among other matters, our historical and projected results of operations, liquidity, cash flows, capital levels, financial condition, debt service requirements and other cash needs, financing covenants, applicable state law, federal and state regulatory prohibitions and other restrictions and any other factors our board of directors deems relevant at the time. In addition, there is no limit on the amount of debt or other obligations we may incur in the future. Accordingly, we may incur substantial amounts of additional debt and other obligations that will rank senior to the securities, which are the most junior securities of our company.
There can be no assurance that we will ever provide liquidity to investors through either a sale of our company or a registration of the securities.
There can be no assurance that any form of merger, combination, or sale of our company will take place, or that any merger, combination, or sale would provide liquidity for investors. Furthermore, we may be unable to register the securities for resale by investors for legal, commercial, regulatory, market-related or other reasons. In the event that we are unable to effect a registration, investors could be unable to sell their securities unless an exemption from registration is available.
The offering price in this offering may not represent the value of our securities.
The price of the securities being sold in this offering has been determined based on a number of factors and does not necessarily bear any relationship to our book value, assets, operating results or any other established criteria of value. Prices for our securities may not be indicative of the fair market value of our securities now or in the future.
Company Information & FAQ’s
The team includes an experienced Medical Director who has a proven track record in the industry and a Digital Health Advisor who is currently the associate head of virtual care for UCSF and actively publishes peer-reviewed research on RPM and virtual care.
Founders also have extensive experience innovating within highly-regulated industries.


Jeffrey Nadel (CEO) and Craig Bolz (COO)
Jeff and Craig are serial entrepreneurs who have founded multiple technology companies, including Klink, Sparkpoint Media, and Beverage Advisory Group. Klink was the first app and website to legally offer on-demand beer, wine, and spirits delivery; had partnerships with Total Wine & More, AB InBev, Nestle, and Constellation Brands; and was acquired by delivery.com in 2017.
They have significant experience scaling businesses and creating partnerships with Fortune 500 companies. Importantly, almost all of their business experience has involved operating compliantly, and innovating, in highly-regulated industries. Jeffrey received his B.A. from the University of Pennsylvania, and Craig earned a B.A. from the University of Central Florida.

Dr. Michael Hafran, MD, MBA (Medical Director)
Dr. Hafran brings more than 15 years of clinical experience and has played an instrumental role in the development of policies, protocols and procedural algorithms ensuring delivery of the highest quality patient-centric care.
Trained in Family Medicine at Columbia-Presbyterian, Dr. Hafran served as a physician and officer in the US Air Force in the European and Pacific theatres. Dr. Hafran has been a strategic advisor and consultant to many different major telehealth and digital health companies.

Dr. Timothy Judson, MD, MPH (Digital Health Advisor)
Dr. Judson is the Associate Director of Clinical Innovations and an Assistant Professor at UCSF. He has expertise in virtual care and telehealth, including remote triage and remote monitoring. He has a passion for designing and implementing care models to improve value and align incentives in healthcare.
Dr. Judson possesses knowledge of various aspects of accountable care organizations and population health. Dr. Judson regularly publishes on the subjects of digital health and remote patient monitoring.

Dr. Andrew Magnet, MD, PhD (Lead Physician)
Dr. Magnet brings over 17 years of hospitalist, emergency room, and primary care experience. He is a physician with hands-on experience, treating all types of patients. He is also the Chief of Medical Staff and a Flight Surgeon for the 165th Medical Group, Georgia Air National Guard.
He graduated from the Medical College of Virginia and completed his residency at Tripler Army Medical Center in Hawaii. Dr. Magnet is a distinguished scholar with his PhD in Molecular Pathology from the University of California at San Diego.

Annie Muehlberger APRN-BC, RN (Patient Care Manager)
Annie is a licensed nurse practitioner who earned her master’s degree in nursing from Walden University and her bachelor’s degree in nursing from Washburn University. She worked as a nurse practitioner for Via Christi Clinic, and before that as a registered nurse for Via Christi Hospital St. Joseph’s Emergency Room.
Our ambition was, and is, to create the kind of healthcare experience that we’ve always wanted our own grandparents to have. Anything short of that is not good enough. We are unconstrained by “the way things have always been done” and are focused on delivering to our patients the best healthcare experience they have ever had.
To get all of the tens of millions of people who currently qualify for, and would benefit from, our service signed up.
By developing the Virtual Care Ecosystem that will power the next decade of healthcare innovation.
Our first mission? Hypertension.
Why? Because nothing kills more Americans than heart disease and stroke.
According to the CDC…
Furthermore, the Surgeon General has issued a “call to action” to control hypertension in America.
According to the report…
High levels of hypertension control can be achieved in clinical settings and communities. Many health care providers—from large integrated health care systems to community health centers serving different populations to individual health care providers—have demonstrated significant improvements in hypertension control in their patient populations and been recognized nationally for their efforts.
They have done so by making hypertension control a priority, implementing evidence-based strategies, and being dedicated to monitoring improvement over time.
These strategies include the following:
We believe our Virtual Care Ecosystem is the answer to this crisis.
Also, by aligning ourselves with existing government priorities, we stand the greatest chance to not only gain market share, but define a new standard of care for the way these conditions are managed.
Based on what we’ve already built, the more participants we have on board, the more we’re able to compile real data. As N gets larger, we think we’ll be able to show the positive impact of our technology.
Assure Health’s medical advisors are standing ready to conduct a full clinical study to definitively demonstrate the effectiveness — and impact — of the Assure Health Virtual Care Ecosystem.
Our top priority this year is running a clinical trial using our Virtual Care Ecosystem and its potential impact on hypertension.
By developing the Virtual Care Ecosystem that will power the next decade of healthcare innovation.
Our first mission? Hypertension.
Why? Because nothing kills more Americans than heart disease and stroke.
According to the CDC…
Furthermore, the Surgeon General has issued a “call to action” to control hypertension in America.
According to the report…
High levels of hypertension control can be achieved in clinical settings and communities. Many health care providers—from large integrated health care systems to community health centers serving different populations to individual health care providers—have demonstrated significant improvements in hypertension control in their patient populations and been recognized nationally for their efforts.
They have done so by making hypertension control a priority, implementing evidence-based strategies, and being dedicated to monitoring improvement over time.
These strategies include the following:
We believe our Virtual Care Ecosystem is the answer to this crisis.
Also, by aligning ourselves with existing government priorities, we stand the greatest chance to not only gain market share, but define a new standard of care for the way these conditions are managed.
Based on what we’ve already built, the more participants we have on board, the more we’re able to compile real data. As N gets larger, we think we’ll be able to show the positive impact of our technology.
Assure Health’s medical advisors are standing ready to conduct a full clinical study to definitively demonstrate the effectiveness — and impact — of the Assure Health Virtual Care Ecosystem.
Our top priority this year is running a clinical trial using our Virtual Care Ecosystem and its potential impact on hypertension.
Dr Hafran: “’We want an N of at least 100, 500 spectacular, and 700 would put us into a true peer review land” The benefit is: As we continue to grow and aggressively expand, our data gets even better, thereby fueling even more growth. We are in a positive cycle.”
We are data doctors. Our goal is to transmit clean and efficient data to the primary care provider that allows for effective change, and to improve quality of life.
Mainly objections would be…
Don’t worry, our physicians will walk you through it. It’s as easy as putting on a shirt
Clinicians might also have objections… I don’t have time to go through this data… don’t worry, we’ll scrub and compile the data, then deliver it to you in whatever form you’d like.
We like to call it the “return of relationship-based medicine.”
We believe in delivering highly-personalized care. We believe in humanizing medicine.
Our patients are not numbers to us — they are real human beings, with all the complexities and nuances that we all share. To best ensure they get, and remain, healthy, we have to strive to understand all of that. And we always do it with a friendly, patient, and compassionate approach.
We are finally providing RPM with clinical integrity. What does that mean? It means that everything we do is in furtherance of the only thing that really matters: keeping our patients healthy. We don’t do things for the sake of technology or for the sake of revenue. What we do, we do to keep our patients healthy. We believe that is a winning strategy.
Unlike other RPM companies, we made the decision to only use fully licensed clinicians and nurse practitioners to render these services because we want our patients to know they’re always in the hands of someone with full clinical decision-making abilities.
While we can’t mention some of our partnerships by name at this time, we have multiple potential strategic partnerships in the works which would contribute materially to our go-to-market approach and speed to scale.
We’ll be announcing these partnerships as soon as they’re confirmed and we have the go-ahead to do so.
Further, we have multiple currently active partnerships with assisted living facilities, home health companies, and primary care providers. Assure Health provides services that these companies can’t or don’t provide themselves, and these services provide tremendous benefit to their clients, patients, residents. In the coming months, we expect to launch additional partnerships with even larger operators of assisted living facilities and senior living communities.
Right now, we partner with assisted living facilities and home health companies to provide more comprehensive services to their patients.
With that said, we’re looking at several other options for channel partners.
Several potential applications here might be:
We have many doors open with respect to potential strategic partnerships, each of which would be expected to result in material impact to the company’s revenue and growth prospects. The company’s founding team has extensive experience in crafting and entering into partnerships with large enterprises, and the founders have a track record of forming such strategic partnerships that dramatically accelerate the growth of the business.
The “secret sauce” of our business is the 20 RPM protocols developed by our chief medical officer.
We have clinical parameters, protocols, decision-making algorithms, and guidelines established to serve over 20 chronic conditions, including:
It is a system that allows for the interpretation of large amounts of data… narrowing it to what is important, and what is not important… then determining how to deal with anomalies and variations that are outside of our safety parameters.
This can be customized for certain patients and allows for a quick, efficient interaction and intervention from our staff.
Our system doesn’t just look at raw numbers. What you want to look at is volatility, delta values, and how people are changing over time.
The real challenge is “how do you separate the signal from the noise?”
You can have a torrent of data, but if you can’t distill it to create action, it’s not useful.
We’ve developed the tools to say what is medically impactful… and where are those decision-making levers… and what should be done.
This is what has not been done before. The clinical infrastructure and algorithms haven’t been put together in a purpose-built way to enable the delivery of these remote monitoring services with clinical integrity.
That’s why there’s always been questionable data — and questions around how that data gets acted upon. And now, we believe we have a solution to this problem.
The Assure Health Virtual Care Platform is built to serve seniors and is especially helpful for those with chronic medical conditions.
Historically, much of digital health innovation has been confined to the benefit of an audience that is relatively young and relatively healthy. Think about wearables like Fitbit and Apple Watch. Innovating for seniors — a population that is older and, on average, sicker — is a much more challenging problem to solve.
But, solving this problem will make the largest difference, as this is the population that drives the lion’s share of costs to the healthcare system and bad outcomes.
Using the Assure Health services to meaningfully help to keep seniors healthy holds great promise on an individual level — improving a person’s health, helping them live longer, etc. — and on a macro level, by reducing costs and suboptimal outcomes.
We do not replace your primary care doctor or specialist. Instead, we collaborate with them to help deliver the best possible care. We are your primary care doctor’s best friend and aim to give them superpowers, in the form of dramatically expanded visibility into how each patient is doing on a much more regular basis.
The traditional model of healthcare delivery in the United States is fragmented and episodic in nature. Patients go to the doctor a few times a year. But that model is not conducive to the effective handling of chronic conditions.
Chronic conditions require active and ongoing management. And when they are under-managed, under-treated, under-medicated, there are numerous bad outcomes that result. For one, patients lose their peace of mind. They are worried between their routine doctor’s visits: “Am I doing okay?” Their family members worry. Time goes by without their knowing if they are getting exactly the care they need.
Ultimately, patients and their families worry about a rapid degradation of their health, condition, and quality of life — the Assure Health Virtual Care Platform is a tool with the potential to help provide peace of mind and reduce the likelihood of avoidable bad outcomes.
Fundamentally, a few of our key differentiating factors are:
We have combined telemedicine with remote patient monitoring to allow for any patient with Medicare to have access to RPM.
We created a hybrid telemedicine-RPM model: Patients have access to RPM services and technologies, with a team of clinicians who monitor their health every day.
Our medical practice specializes in RPM services: All clinicians rendering services are specially trained and experienced not only in rendering care remotely, but also in the specifics of monitoring physiologic parameters on a regular basis and communicating with patients accordingly.
One of the really incredible things that we are able to do is personalize this based on what the patient needs. We provide at least one patient interaction per month, but it could be as often as what is required and medically appropriate on a per-patient basis.
We have sourced and developed technology that makes both RPM and telemedicine easy to use for seniors.
All of the devices we use include embedded cellular modems so the data is automatically transmitted into our EHR without the patient doing a thing.
We prepare and pre-provision each device before shipping to patients so everything works right out of the box, and we do not require any app downloads.
We use a unique technology infrastructure, bringing together existing technologies along with our own proprietary tech stack that enables us to deliver an unrivaled, seamless experience.
If a patient requests automatic PCP data sharing and signs a HIPAA release, then we can do this automatically. If they do not request it or do not sign a HIPAA release, PCP collaboration will only occur during escalations.
We also have patients who do not request automatic sharing, but request it as-needed prior to their appointments with their PCPs.
Yes. The devices “phone home” when working properly. As long as you have cell phone coverage, this technology will work for you.
There does exist the potential for international expansion in the long-term, but, for the foreseeable future, we are completely focused on the U.S. domestic market. Our expansion will take the form of expanding our scope of services far before we look to international expansion.
Yes, we do have customers. Our current patients were acquired through a two-pronged approach, including both pure direct-to-consumer efforts (e.g., direct response marketing) and channel partnerships (e.g., with assisted living facilities).
Based on Assure Health’s current legal status, our licensed medical providers can offer services to patients in Florida, Alabama, Delaware, Georgia, Louisiana, Maine, Mississippi, Missouri, Nebraska, Ohio, Rhode Island, Utah, Virginia, and Washington, D.C.
However, Assure Health is currently in the process of expanding its reach to all 50 states, a process which is expected to be completed within the next six months.
Our average CAC for December 2020 was $67.50.
We have built our systems and processes to scale to 20,000+ patients.
We bill Medicare and private insurance companies.
The Assure Health model has high retention, which we have already demonstrated, due to the relationship-driven nature of the services and how integral they become in patients’ lives. While services are only delivered so long as they are medically necessary and appropriate, we have found that most patients are in need of long-term remote patient monitoring for their conditions.
For our financial modeling, we estimate an average of $130 in monthly revenue per active patient. This estimate is based on national payment amounts from the Medicare Physician Fee Schedule.
All medical services provided to patients are based exclusively on the medical necessity and clinical appropriateness thereof, as determined in the sole discretion of the licensed medical professional(s) rendering services to the patients in question. Our average “days to pay” from Medicare for Q4 2020 was 17.5 days from the submission of a claim to the payment of a claim.
Based on Medicare’s national payment amounts from the Medicare Physician Fee Schedule and industry-level cost data as well as our own data, gross margin is projected to be in 50%+ range.
Between August and December, we increased our number of new patients onboarded per month by 160%.
In addition to the value that the business drives and the pain points it solves, the timing for our solution could not be better. As COVID-19 has gripped the world, droves of people — especially seniors — who had previously never used telehealth services have flocked to these offerings.
Now, it can be very dangerous for members of these at-risk patient populations to leave their homes; a doctor’s waiting room may be the worst place for them to be.
As a result of these macro trends, there is an intense focus on telehealth and digital health solutions and a corresponding desire to adopt them.
The knowledge that investors are helping to fuel a company that is contributing to preventing hospitalizations, catching patients’ issues before they become major, and ultimately saving lives, along with significantly reducing the long-term cost burden of chronic conditions on the healthcare system.
We expect the company to become cash flow positive at a very early stage considering the strong profit margins and LTV of our patients. As a result, the company will not need large amounts of ongoing funding.
However, we acknowledge the importance of establishing ourselves as the market leader in this space and spending to acquire large numbers of patients quickly. Fundraising will buy us speed.
There are many avenues for liquidity in our space, from acquisition opportunities by large legacy players to public market opportunities, all with the aim to enable our growth and achieve our vision of “A Doctor in Every Home, at no out-of-pocket cost”
communication forum
You must be logged in to post a comment.
The next 8 slides will allow us to process your investment. Note that these next steps are a legal requirement – Thank you for your patience and financial support of this investment opportunity. Jordan Gillissie – CEO
Before we execute the investment, it’s important for us to make sure you’re comfortable and knowledgeable in early stage investing. We want to make sure that you:
We are currently upgrading our system. If you click submit and the process does not continue in a few seconds, please refresh this page manually, and click Invest Now again and you should be moved on to the next step.
Please wait a few minutes while we create your account. An email will be sent to you shortly to confirm your admittance. Should the email be delivered to your spam or promotions folder, we recommend you move it to your inbox and mark Equifund as a safe sender.
If you have not received the email in 5 minutes, please click here to have it resent.
Questions? Our customer service team is always here to help – 1-866-338-3004
Hello. I have a few questions.
-What was your 2020 revenue?
-What are your revenue goals for the next 5 years?
Do you ask for the patient’s PCP info and relay potential health issues to them when detected?
Also, please elaborate on your device:
-Does it cost anything to the patient?
-How many different devices are there? I think I only saw the blood pressure on the video.
Thanks in advance.
Hi Leonardo! We appreciate your questions and interest in Assure Health!
First, regarding your question about coordinating with a patient’s PCP — Yes, this is a hugely important part of what we do. When patients are onboarded, we always ascertain the names and contact information of the patient’s PCP and any other specialists who are helping to manage their conditions. We then have a collaborative relationship with a patient’s other doctors. Our founders like to say that we give the PCP “superpowers,” because we may provide them with a higher degree of visibility into how a patient is doing on a daily basis — and when any problems arise — than they otherwise would be able to have. Any time an escalation necessitates PCP involvement, the PCP is involved right away.
Second, to your question about cost to the patient — This is dependent upon the patient’s insurance coverage. We do not “sell” the devices to patients. Rather, the devices are provided for a patient’s use during their participation in physician-ordered remote monitoring services. So the cost to the patient is completely based upon their insurance’s coverage for these services. Many of our patients pay $0 out-of-pocket for the services and devices because remote monitoring, when medically necessary and properly administered, is often covered by Medicare and other insurance providers. We are committed to price transparency, so we always run a check on each patient’s insurance upfront so that we can let them know if they will have any out-of-pocket financial obligation before they move forward with the services.
Third, to your question about the number of devices — As of today, we make use of three different devices: (i) blood pressure, (ii) body weight, and (iii) blood glucose. We are constantly adding new devices and are engaged in deep R&D on new technologies we can implement over the coming months and years.
Fourth, to your question about revenue and projected revenues — Due to the sensitive nature of revenue projections and our compliance responsibilities with respect to SEC regulations, we’d encourage you to read through the offering page above as well as our Form C, which is linked to from this page. In addition, Equifund should provide you with an independent valuation report, which includes further detail on revenue projections.
Thanks so much!
Greetings!
– We also would like to know the level of tech literacy that is required to function in your ecosystem?
– Could an authorized family member have access to real-time data? Such as heartbeat to know the parent is okay?
Hi Daniel! Thanks for your questions and your interest in Assure Health. More than happy to jump in here and provide answers.
First, to your question regarding tech literacy. We put every single patient-facing piece of our ecosystem — from the medical devices we use to capture physiologic data to the telehealth technology we use to support the audio/video appointments — through what our founders always call “the grandparent test.”
Each of our team members is always encouraged to pose the question to themselves, and to the rest of our team: “Would my parents or grandparents have any difficulty using this?” If the answer is yes, we always go back to the drawing board and try to figure out another way.
In short, we have tried to keep the level of tech literacy required to participate to an absolute minimum. For example, the medical devices we use couldn’t be simpler. Patients simply pull them out of the box and start using them, taking their blood pressure, weight, glucose, etc. They don’t have to worry about Bluetooth or wifi. Every time they take their numbers, the devices use an embedded cellular modem to wirelessly transmit the data to our clinical team, without any further action on the part of the patient.
We’ve gone to great lengths to make sure that someone who is not particularly adept at technology, doesn’t know how to pair a Bluetooth device, doesn’t want to download a mobile app, etc. can still sign up for Assure Health and derive the benefits.
Second, to your question about authorized family members having access to a patient’s data. This is such an important part of what we do! When we talk to patients and their families, one of the phrases we hear again and again is, “peace of mind.” Assure Health is often able to deliver to patients and loved ones alike a degree of peace of mind that is otherwise really difficult to find.
We are incredibly privacy-conscious, and we abide by HIPAA to always ensure we keep patients’ personal health data private and secure. As long as a patient provides the necessary HIPAA consent, we can share data with a patient’s family members so that they know their loved one is doing okay. Further, we always ask patients if they have certain family members they’d like to be notified in the event that we have an escalation due to elevated or problematic readings.
Thanks so much!
First off, this is one of the better presented deals that I have experienced. Hats off to you and Equifund.
What competitors do you have in the RPM space that currently have sign up options thru Medicare?
What is your new customer acquisition goal for a hypothetical raise of the maximum target for this offering?
The large part of your service is the personal interaction between medical practitioners and patients. The personnel are not employees of Assure but contracted by a third-party.
Is there a system to monitor personnel or at least a process/training set up on how to interact with patients as they represent Assure?
Thank you in advance.
Hi Eric — We really appreciate the kind words! Along with the Equifund team, we’ve worked hard to try to ensure we pack in as much information we can about the company and our plans, so this means a lot.
We’ve jumped in and provided answers to your questions below:
+ Right now, to our knowledge, we do not have any direct competitors taking the same approach as we are in the market. Our most important differentiated advantages are (i) our direct-to-consumer pathway that we’ve built for directly onboarding interested patients, and affording those with certain insurance coverage the ability to access the services without significant financial burden and (ii) our purpose-built clinical infrastructure, specifically built to allow for the remote monitoring of 15+ chronic conditions, with clinical integrity. Others in the market have not tackled — and solved — these critical problems.
+ Our goal is to acquire around 4,000 new patients using the proceeds of this raise.
+ You are absolutely right that, given the critical importance of human relationships and personal interaction, ensuring quality is a top priority of ours. Our plan is for all nurse practitioners working with Assure Health patients to be 100% dedicated, working full-time exclusively with Assure Health patients. Also, even though we leverage independent medical professionals and practices, pursuant to state corporate practice of medicine laws, we provide administrative, management, recruiting, and other staffing services to these practices to aid in quality assurance and uniformity of service, though we do not direct the clinical practice of medicine.
+ Yes, we have in-depth training and quality assurance protocols in place, including robust clinical protocols, parameters, and clinical decision-making algorithms, in order to ensure the highest possible standard of care. We also have extensive monitoring and quality assurance methodologies available to us.
Thanks so much!
Hello,
I can’t find the company’s website. Would you please reply me it? Thank you.
Hi Branden! Absolutely. You can find the website at http://www.myassurehealth.com. Thanks for your interest!
Very good presentation and I am all for reducing the healthcare cost and the deficits we pass on to our children while reducing “waste” and enhancing the patients care using technology. Have few questions.
1) Is your revenue mainly comes from the monthly subscription dues (e.g. $130/mo used in the multiplier valuation projection)? OR are there any additional sources also?
2) How many patients currently on your platform?
3) What is the patient acquire cost? What is your monthly run rate to sign up new patients and what is the retention rate?
4) What IP and other proprietary value you hold that can not be easily replicated by competitors?
Thanks for answering these questions.
Hi Girish! Thanks so much for the positive feedback. We agree that it couldn’t be more important to reduce the costs of healthcare while doing everything we can to improve quality and outcomes. The opportunity to do this is one of the main reasons our founders started Assure Health.
Let me address some of your questions below:
We receive revenue primarily on a recurring basis for the remote monitoring services and devices we provide. The lion’s share of this comes from insurance payors, limiting the out-of-pocket financial responsibility to individual patients themselves. There are a few other sources of revenue as well, including from telehealth visits between physicians and patients. Over time, we are confident that there are many ways to expand the scope of services and increase revenue as well, but we have established a solid foundation of recurring revenue with sound unit economics. Our most recent measurement of average, blended patient acquisition cost was around $67, and the patient retention rate is upwards of 92%. We have gone to great lengths to develop proprietary value to differentiate the Assure Health solution. One of the most important aspects of this differentiation are our clinical protocols and parameters developed specifically for clinically robust remote monitoring of patients with chronic conditions, which were developed by our Medical Director. In addition, have developed — and are continuing to develop — technology that aids in the delivery of these care services in a way that is not served by current EHR and similar technologies, including by providing for the streamlined aiding of providers in clinical decision-making.
Thanks so much!
Hello,
That was a well put together presentation, Thank you that.
You spoke of the need to service patients in rural areas however I believe we would be considered remote with having no cellular service in the mountainous terrain we live in.
We currently only have access to the internet via through satellite and land line DSL services. With your equipment being wireless is it capable of working with an at home network and transmitted out through the internet?
Thank you
Hi Guy! Thanks for the question and for your interest. This is important, as expanding access is one of our most significant goals, and this goal is especially important in the context of rural communities where folks may have less frequent access to in-person medical care.
Right now, our devices have embedded cellular and do not work on wifi. We made this decision early on to optimize for usability. Bluetooth and wifi presented too many problems, with folks in our patient population having to figure out how to pair and configure these devices. Instead, we opted for devices that just work right out of the box.
The devices are able to make use of newer technologies, such as those leveraged by connected Internet of Things devices, which use narrow band M2M frequencies. While reception in a given area may not be sufficient to make a phone call on a normal smartphone, there is often still sufficient reception at these frequency bands to transmit the small amount of data we require. For more information, check out this article, which we found interesting: https://www.gsma.com/iot/narrow-band-internet-of-things-nb-iot/. The technology we use also connects to the local cellular network with the optimal coverage in a particular area. We are also working on adding wifi-based devices in the future to help address this use case.
Thanks so much!
How do you test for blood glucose? Does the patient have to draw blood?
There’s nothing about revenues in your Form C or anywhere in the offering page. I’m not asking for projections, just your personal revenue goals/targets for the next 5 years. That would give me an idea of the company’s growth potential.
Thanks again.
Hi Leonardo,
Thanks for the follow-up questions! The glucometer is a traditional finger prick test for blood sugar, with one important difference: after each reading, the data is transmitted remotely, without further action from the patient, to our clinical team via a cellular connection. We are also working on adding continuous glucose monitoring (CGM).
We estimate that the addressable market in our target population for remote monitoring services alone is approximately $50B annually, with solid growth as well. Our goal is to hit an annual revenue run rate of at least $50m in the next 3-5 years.
(Certain information contained in this answer may constitute “forward looking statements.” Furthermore, any forecasts or other estimates in this answer, including estimates of returns or performance, are “forward looking statements” and are based upon certain assumptions that may change. Due to various risks and uncertainties including the risk factors described in this answer and the accompanying offering materials, actual events or results or the actual performance of the securities may differ materially from those contemplated in such forward looking statements. Moreover, actual events are difficult to project and often depend upon factors that are beyond the control of our company. These statements are not guarantees of future performance and undue reliance should not be placed on them. Such forward-looking statements necessarily involve known and unknown risks and uncertainties, which may cause actual performance and financial results in future periods to differ materially from any projections of future performance or result expressed or implied by such forward-looking statements.)
Hi
I read that on the Equifund website that Jeff and Craiq were the co-founders of Sparkpoint. I was trying to read about Sparkpoint. However, the link to the site does not seem to be working. Is this company still functioning?
https://www.sparkpointgroup.com/
Thank you
Kurian
Hi Kurian — We appreciate the question! Sparkpoint was a joint venture founded by Jeff and Craig in the beverage alcohol technology space with several significant partners, including a publicly traded company. Sparkpoint created the first legally-compliant way for brands in the beverage alcohol industry to advertise in a digital, interactive way in-store. The branding of the company changed over time as certain functions of the business were taken on by the joint venture partners. Jeff and Craig also previously founded Klink, which was acquired by delivery.com: https://www.miamiherald.com/news/business/article144161594.html. Thanks so much!
Two questions:
1. How do you ensure HIPPA compliant?
2. Cybersecurity: What steps do you have in place to reduce the likelihood of internet security breach, client information exposure, ransom ware, etc?
Thanks,
Peter Young
Hi Peter! We really appreciate this question, as data privacy and information security are of paramount importance to us. We go to great lengths to ensure that we are protected and compliant on this front. We employ the services of a Chief Information Security Officer, who helps us draft and enforce information security policies, and we have many such policies in place, governing everything from the use of passwords to the security of physical premises and the shredding of hard-copy documents. We leverage encryption, backups, password protection, and other industry-standard measures to ensure we remain safe and in compliance. We have even begun going so far as to ensure that we have the ability to remotely wipe and disable all employee devices and immediately disable access to accounts. We also have clear policies in place for obtaining patient consent for any sharing of health or other personal data. Assure Health also enters into Business Associate Agreements, per HIPAA, with vendors and partners who interact with health data, to ensure compliance and security. Thanks!
Hi, are you planning to allow investing for non-US citizens as well? If yes, when? Thank you, Attila
Hi Attila! Thanks so much for your interest! Unfortunately, at this time, investment is is limited to U.S. investors. This is due to the regulations that are in place and the compliance burden involved therewith. We certainly hope to be able to accept international investors in the future, and we’d encourage you to reach out to Equifund to find out if, and when, they will be able to allow for international investors in the future.
How much investment are you trying to raise this round?
Hi Peter! Thanks so much for your question! We are currently raising a maximum of $1,000,070, which is the current limit imposed under Regulation Crowdfunding.
The equipment that you guys send out to the patients to help monitor their medical status, will this be charged for or is this free with the monthly charge?
Thank you very much
Hi Aurus! Thanks so much for your interest and for your question. This is a common question, so we really appreciate your providing the opportunity for us to offer some additional detail on this. The devices are provided to patients for the purpose, and for the duration, of their participation in the program. For patients whose insurance provides coverage for remote patient monitoring, the use of those devices is generally included in the amount covered by insurance. We do not sell the devices directly or “charge” for them in any way other than through participation in the clinical services. We hope this helps and makes sense!
Great briefing !! Congrats for raising so far and hope to hit Maximum soon. Have some questions
1. Why crowd funding
2. Are the devices proprietary to AssureHealth or its out of box 3rd party devices
3. Can you justify valuation
4. Is it targeted only for Medicare? Would there be possibility for retail service in future? International market possibilities?
Thank you for the kind words, positive feedback, and great questions! We have provided answers to your questions below:
1) Why crowdfunding?
We decided that we want to build a community of shareholders who all have a vested interest in our success. There are so many synergies that we have already observed with this community. For example, we have investors who are doctors and other healthcare professionals who are making introductions for us, providing suggestions, and helping to push the business forward in other ways. We also have investors who have reached out to become patients themselves. Overall, we loved the idea of having a community behind us who could help to evangelize Assure Health and connect the dots to potential patients and partners.
2) Are the devices proprietary to Assure Health?
As of today, Assure Health is not a manufacturer of medical devices. Rather, we exhaustively source the very best third-party medical devices we can possibly find, settling only on those that offer the most seamless, frictionless experience possible for patients. We are also engaged in various R&D projects involving the use of new technologies to generate and transmit physiologic data, which are being conducted in-house and would be proprietary.
3) Can you justify valuation?
We engaged with a third-party solution to prepare valuations using multiple different methodologies. There is a third-party report that can be accessed through Equifund. We also had significant investor interest at this valuation.
4) Is it targeted only for Medicare? Would there be possibility for retail service in future? International market possibilities?
We are currently focused on the 65+ senior population, principally those with chronic conditions. We see that area as being the biggest driver of need at this time. Patients can use any insurance, including Medicare, that provides coverage. In the future, we absolutely think there is an opportunity to partner with private insurance companies (in addition to the existing, primarily Medicare-driven patient population) as well as international health systems.
How can Canadian investors participate. The portal seems to only accept US located investors.
Hi Kwasi! Thanks so much for your interest! Unfortunately, at this time, investment is is limited to U.S. investors. This is due to the regulations that are in place and the compliance burden involved therewith. We certainly hope to be able to accept international investors in the future, and we’d encourage you to reach out to Equifund to find out if, and when, they will be able to allow for international investors in the future.
Hi was wondering when your plans are to go public with this? aka getting on the stock market with a ticker number. Can you please advise regarding the timeline.
Hi Anfisa! Thanks so much for your interest and for your question. At this time, this Reg CF offering is the only way for members of the public to invest. We will absolutely keep you apprised of any and all updates to the company as we progress further.
Are you planning to do a rolling close?
All the best with your funding!
Few questions:
1. I understand that your goal is to hit 20k patients. I am doing some math here based on the call we had today. @ 1 nurse per 200 patients, would you be able to staff and maintain 100 fulltime nurses on payroll. This seems to be akin to a small hospital.
2. You mentioned a Gross margin of 50%. If i assume 20K patients @ annual revenue of 31M USD. ~25% of this revenue will go to paying salaries of 100 nurses. Run cost of devices, replacements, cost of clinicians, will take up a some of the revenues. Do you have a high level breakup that you can share that arrives at 50% margin.
3. I read above that there is an independent valuation report. I cant find it in the site. Can you share that or point me to the document.
Thank you
I was able to listen to your Corporate Update with Equifund. The information was good and encouraging. A lot of discussion dealt with scaling. Unfortunately, I didn’t hear any information on being able to offer services to all 50 states. How is this process going? Are you still on track to achieve offering your services in all states in about four months?
Hi Eric! Thanks so much for joining us for the Corporate Update; we really appreciated the opportunity to do it. Yes, we believe we are still on track for that timeline. Given how we’ve set up our corporate structure, it’s largely just a matter of some additional legal fees and paperwork. We are making great progress and expect to have nationwide coverage within a few months.
If you are unfamiliar with InnaMed, it would be worth your while to check them out. They are a startup developing a home blood testing device with remote reporting that you might use to expand your services. They are currently raising on Wefunder.
Thanks so much for sharing this with us, Timothy! We will absolutely working with our Medical Director to look into this. If we are able to validate it, yes, you’re absolutely right, there could be quite a lot of synergies; it looks like a tool that could potentially allow us to serve patients even better. Really appreciate your suggestion!
Reposting my earlier comment/ question as I did not get a reply as yet.
All the best with your funding!
Few questions:
1. I understand that your goal is to hit 20k patients. I am doing some math here based on the call we had today. @ 1 nurse per 200 patients, would you be able to staff and maintain 100 fulltime nurses on payroll. This seems to be akin to a small hospital.
2. You mentioned a Gross margin of 50%. If i assume 20K patients @ annual revenue of 31M USD. ~25% of this revenue will go to paying salaries of 100 nurses. Run cost of devices, replacements, cost of clinicians, will take up a some of the revenues. Do you have a high level breakup that you can share that arrives at 50% margin.
3. I read above that there is an independent valuation report. I cant find it in the site. Can you share that or point me to the document.
Thank you
Hi Kurian, apologies we missed your initial question. Have replied below:
1) We believe that one nurse practitioner per 200 patients is a conservative estimate. We think that leveraging medical assistants for non-patient-facing tasks and similar optimizations can significantly expand the amount of patients a Care Manager can provide care for. It is certainly true that as the business scales, we will need to have significant headcount on the clinical side because that is a major component of the service we offer; we view this as an asset, not a liability, as we are building a business premised upon delivering excellent service with a foundation of human relationships.
2) The calculus of the 50%+ margin includes device cost amortized over the course of 24 months, clinical labor, and projected device replacement.
3) The valuation report can be accessed on Equifund by creating an account. If that is not working, they can provide over email at [email protected].
Thanks so much!
One Assure health has raised the target funds, what is the projected timeline for reaching IPO?
What other companies are in this market space and what differentiates your service/value from theirs?
Attention shareholders and prospective investors: Assure Health will be closing its Regulation Crowdfunding offering on June 21, 2021. We’re excited to report that since we launched our Regulation Crowdfunding offer on Feb 15, we have had a handful of major successes. These successes include adding several key members to our team, In the process of partnering with a major American academic health system, and most importantly, signing a contract with a national player in the healthcare space. This player processes over 1 million patient touch points per week and will dramatically increase our ability to scale customer acquisition. The deal will also serve as a springboard into other key relationships with household brands. Because of these developments, we strongly feel the current $10.687 million million valuation greatly undervalues the company. As such, we have decided to close our Regulation Crowdfund offering early on June 21, 2021. If you are considering an investment, please be aware that is the final date to invest. We will not accept new investors in this offering after June 21, 2021. This raise with Equifund has been a great success and was a big factor in enabling us to achieve key milestones in a few short months. We would like to thank everyone that participated and to welcome all new shareholders as we progress toward our goal of becoming a billion-dollar company.
Hi Assure Health Team,
I have read through your whole presentation and the questions posted by investors on Equifund. You have a very compelling vision and workable approach to fulfill this vision! I like your company very much and am considering investing in it.
I have a few questions:
1) Almost all of your leadership team (listed in your presentation and your company website, and cross-checked with LinkedIn), except the COO, are part-time. Even the CEO is part time; he is also the CEO of Sparkpoint and Principle & Founding Partner of Beverage Advisory Group. This is worrisome. How will this be changed going forward, especially when you scale, particularly with your signing of a contract with a national player in the healthcare space? Surely this conversation must have come up in your contract negotiation with this national player.
2) As of now, you have not done a full clinical trial yet. In the FAQ section of your presentation, you stated, “Assure Health’s medical advisors are standing ready to conduct a full clinical study to definitively demonstrate the effectiveness — and impact — of the Assure Health Virtual Care Ecosystem.” And Dr. Hafran stated, “We want an N (participants) of at least 100, 500 spectacular, and 700 would put us into a true peer review land.” Do you still plan to conduct this trial? Surely this conversation must have come up in your contract negotiation with this national player.
3) Does this contract with this national player place you over your stated 20,000-patient goal at the beginning of your presentation (“… this breakthrough business model could create the next “MedTech” unicorn with only 20,000 active patients”)? By a wide margin?
Thank you in advance for answering my questions!
John Hwung
Hi John. Thanks for your questions! We appreciate your kind words about our vision and approach — and your consideration of becoming an investor.
To address your questions:
1) All of our core team is full-time, including our CEO. Most of our team works full-time from our headquarters in South Florida.
2) Yes, we are still very much planning to conduct the clinical trial. And we have had very positive early indications of positive outcomes.
3) We want to be careful about making concrete, forward-looking predictions like that, but we are optimistic that the deal represents a quantum leap for the company and for the company’s ability to scale.
Hi Samuel Lennox here I am already a piece of the company, I would like to speak to Mr Nadal or Mr Bolz about getting on the monitoring program, see Sir I was involved with the company by Equifund, when I read what the company was doing I asked to include me to the company, then Chip call me because I was a member of Medica health care I gave him my phone number and my Medica ID # 2hr later he said I’m not qualified, I’m qualified because I call United Healthcare and it takes me 3 days on the phone on hold for 1-2hrs I use all the minutes on the phone it takes 2 days to get minutes back on the phone he try to call I try to call nobody knows who Chip is, now everybody wants to sign me up I said no I need to talk to Chip days after one guy say he’s on the phone he’ll call me back nothing happened ,anyway I was clear after calling Dominican Republic and Colombia, Then these 2 companies sign me up for themselves I said no I’m already with Assure Health, so I call Equifund and ask them for the phone number. Please let mrJeffrey Nadal call me @7549461207 the story gets sweeter I’ll tell you the rest of it when we talk thanks Sam Lennox.
I am invested for the minimum and would like to add funds before the upcoming deadline. What is the incremental minimum add? Please respond promptly.
Michael P. Gretchen